What’s this at the end of my toe
Causes of painful toe swelling
Curious shapes, distortions and nail problems are always fascinating to podiatrists. Facebook produced a series of questions recently from podiatrists and there I decided to update this article.
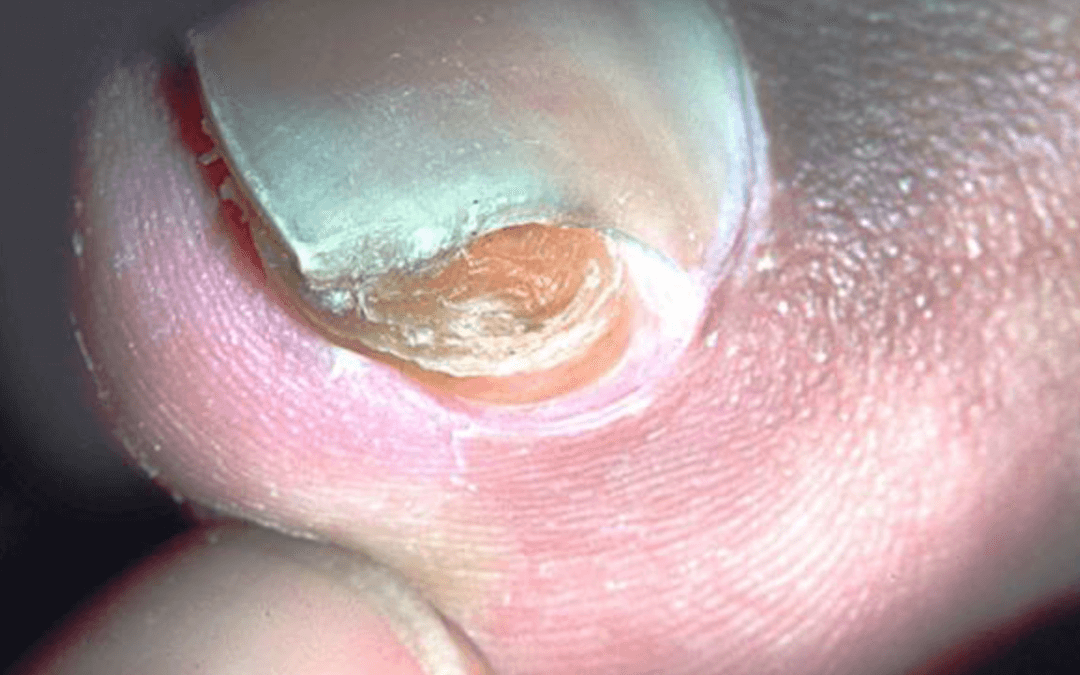
Ivan Bristow published an article on Why does my toenail hurt? You can download this using the link below. This is not the first article that has caught my eye from Dr Bristow and you can read another article on Pilonidal Sinus as part of my Footlocker series. The cover photo is courtesy of Dermatology Advisor (click here) and is a useful resource for podiatrists and people with a deeper sense of enquiry. I draw on my own experience after 32 years as a podiatric surgeon. The distortion of the end of the toe and callus formation in some of my patients was not uncommon and I had to treat this together with what we call the nail apparatus. The term collectively involves the nail bed. A red hard swelling was evident in young patients, usually under 30 years of age where the nail was often thin and heavily distorted.
If it looks suspicious it probably is not right, but that doesn’t mean it’s malignant!
Ivan’s own observation is thus quoted…
A painful toenail in an adolescent or young adult with accompanying nail changes may suggest the presence of a sub-ungual exostosis. The exostosis is typically an osteocartilaginous tumour of the distal phalanx. Visually, one may observe a red nodule in the early stage under the nail which may protrude from the free edge which is solid to the touch but blanches under pressure. As it grows localised distortion of the toenail can occur with symptoms such as involution or onychocryptosis which may disguise the diagnosis.
 Ivan’s article can be downloaded and covers glomus tumour, sub-ungual corn, the subject of this article, osteoid osteoma and of course exostosis. But what is an exostosis and what does sub-ungual mean?
Ivan’s article can be downloaded and covers glomus tumour, sub-ungual corn, the subject of this article, osteoid osteoma and of course exostosis. But what is an exostosis and what does sub-ungual mean?
Exostosis is an abnormal outgrowth of bone while sub (under) and ungual imply the tip of the toe. Ungulates such as horses walk on the tips of their toes and their nails have adapted into a single bone and toenail, the keratinised hoof.
Finding more information
 There is a dearth of material from some of the formal UK sites but the NHS and Wye Valley NHS Trust had written a specific guide sheet available to download here (guide sheet). When it comes to factsheets and guides one certainly finds great variations and there is no doubt if you perform a search you will find more information, often from the USA. Bristow’s article and Dermatology Advisor are valuable. To read more about fact sheets and what makes a good factsheet click here.
There is a dearth of material from some of the formal UK sites but the NHS and Wye Valley NHS Trust had written a specific guide sheet available to download here (guide sheet). When it comes to factsheets and guides one certainly finds great variations and there is no doubt if you perform a search you will find more information, often from the USA. Bristow’s article and Dermatology Advisor are valuable. To read more about fact sheets and what makes a good factsheet click here.
What is it and why is it confusing?
 The condition seems to be limited to the young because of immature cells being involved. We know that chondrocytes can change to osteocytes as part of growth development and chondrocytes are the name given to cartilage cells. This is the soft material that you find on the ends of bone joints with raw meat and chickens.
The condition seems to be limited to the young because of immature cells being involved. We know that chondrocytes can change to osteocytes as part of growth development and chondrocytes are the name given to cartilage cells. This is the soft material that you find on the ends of bone joints with raw meat and chickens.
An injury to the toe is common, not least because the toe sticks out at the end of the body. The excessive growth, like hyper granulation in an ingrown toenail confuses the clinician because the skin is shiny, stretched, red and easily knocked. I always sent off my samples of bone once removed at our local hospital, for some years, and they used a specialist hospital in Glasgow to peer review any interpretation. I knew that elsewhere in the body the bone-cartilage lesion known as an osteochondroma could become malignant in <5% of cases, but as far as the foot was concerned this was something that I never saw
My youngest patient was 10 years of age and the average patient was probably around 19-20 with the oldest osteochondroma at 35 years. I have seen pseudo exostoses, little spikes in all ages but the subungual osteochondroma forms thickened skin that looks odd, as it has blood vessels running through. This can be confused with angiokeratomata. These are defined in an article by the Primary Care Dermatology Society (PCDS).
Again the skin with its blood vessel distortion and raised nail edge can be caused by the end of the toe bone sticking out with cartilage capping over the end (see Figure 1 below), where the skin is stretched. Illustration A shows the nail distorting type of exostosis, or subungual projection distorting the nail, while B shows the smaller phalanx of a lesser toe projecting abnormally forwards. The red areas indicate stretched skin and in the case of A, the nail may appear soft, thin and moulded.
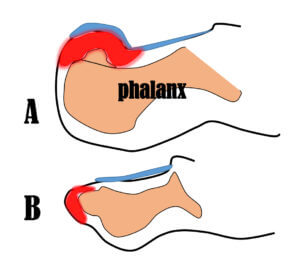
Figure 1. Two scenarios. Subungual exostoses are often associated with osteochondroma. Nail in blue. Skin stretch red. Bone pinky-orange
Planning & Treatment
Radiology is mandatory. That ever-increasing passion for debridement should be resisted as the skin will bleed easily. A healthy suspicion of cartilage must be considered in younger age groups. There is no need for a biopsy (sample specimen) if surgery is being performed as radical excision (cutting out) is necessary with nail bed repair afterwards.
More often the nail will return only slightly damaged after surgery, but all patients must be made alive to the reality that the nail may be permanently thickened, discoloured or distorted. This can be dealt with later by permanent removal. Guide sheets, such as the one produced by the Wye Valley podiatric surgery department, will inform patients what to expect and how to best recover after surgery.
- For the patient any swelling should be examined by a professional if it is slow-growing and no notable injury is attributed
- Wear open-toed footwear until you can see someone or as deeper toe boxed shoes as possible. Soft uppers might be better to avoid pressure.
- For the podiatrist or GP. Take an x-ray if suspicious and act upon the findings
- The lesions are rarely malignant but should be treated with moderate urgency to seek an early diagnosis from excisional biopsy
- All surgical treatment should come with a fact sheet and post-operative guide
- Surgery is suited to local anaesthetic management in appropriate facilities
- Histology is always advised with this the osteochondral lesion but such decisions will be based on the surgeon’s experience and local policy
Should a patient be seen by any other specialists? This will depend on your local area, those who have appropriate training and experience in foot surgery are the people to discuss treatment with. If in doubt speak to your own GP as to who to see in your area but it is important to make it clear that you are trying to rule out malignancy and delay should be avoided. After the effects of covid, it is difficult to predict the speed of referrals onward but a direct referral to a specialist is much preferred and this is where a quality referral letter is required.
Thanks for reading ‘What’s this at the end of my toe?’ written by David Tollafield
Sign-up for here my regular FREE newsfeed
Why not read – Podiatry as a career choice?
You can also read other articles produced for ConsultingFootPain
Published by Busypencilcase Communications Est. 2015 for ConsultingFootPain


Recent Comments