Ultrasound in focus and Podiatry
Reflective thoughts and evidence around ultrasound
Ultrasound within podiatry is the theme of this article. All professionals will inevitably extend their ability as part of professional development. This is often known as extending one’s scope or range of skills. Opposition to expansion arises for different reasons. Lack of confidence by a greater majority can impede change. Strong views are held in respect of what is viewed as traditional scope. A need to stick to what we learned at university. There is no doubt that those that offer indemnity cover have their own views as to risk. When it comes to ultrasound there is a storm brewing. It is one that is as old as time. The real question will be how much regulation of ultrasonography should there be?Commercialism plays a strong part in how scope may develop. Qualification does not always come into the equation as identified in a study undertaken and published in JFAR 2018. Siddle HJ et al emphasises one view.
‘Unfortunately there is no legal requirement to hold recognised ultrasound qualification in order to practice as a sonographer in the UK…’
On the surface this is a reasonable and responsible statement which doubtless aims to provide protection of the end user – the patient. The Health and Care Professions Council (HCPC) do not recognise a need (presently) to ensure that users are accredited with a formal course. One might ask how many podiatrists have undertaken any training. Perhaps this is where we meet some uncertainty because there are many forms of ultrasound. Broadly these break down into three key categories. Then there are localised injections.
Use of ultrasound in podiatry
Therapy
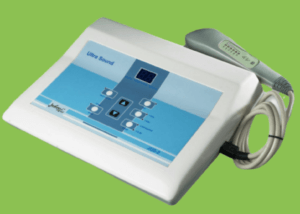
Pictured on e-bay
Ultrasound used as a traditional physical therapy to assist soft tissue problems make up the greater bulk of these activities. Siddle’s paper informs us that 11% (32/284) used therapeutic ultrasound. Tendon conditions were the most frequent area of concern. There are a wider range of ultrasound units sold without any regulation in regard to equipment. This is often seen commercially branded as ‘pain’ management. Electrical pulsed equipment has also been marketed for wide sale. In regard to the foot there has always been a question around its value and Extracorporeal Shock Wave ECWS has to some extent overtaken the popularity of therapeutic ultrasound. The key targets are helping patients with fascia, tendon and heel pad pain.
Vascular diagnostics
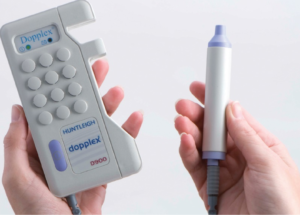
Huntleigh catalogue picture
Handheld Doppler ultrasound provides an audible auscultation method to determine the quality of blood flow in veins and arteries. It is cheap to purchase. It supports the use of palpation to feel pulses such as femoral, popliteal, peroneal, tibial and dorsalis pedis arteries depending upon the set frequency of the head of the probe. Undergraduate training will achieve adequate competencies as it would for therapeutic case management. In many cases this is part of the objective structured clinical examination or OSCE system for student assessment. Siddle found 40% of their respondents has completed ultrasound training as part of their undergraduate degree programme. The more expensive vascular flow machines are less attractive to podiatrists outside the NHS such as Duplex ultrasound which is a more sophisticated system than the simple handheld Doppler.
Sonographic imaging
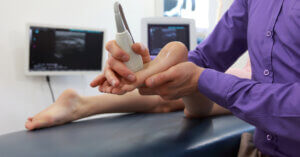
Extending the scope of podiatry causes concerns over training
A third group relates to sonographic imaging. Sonography differs from the other two categories as it has a dedicated profession with an educational framework. While the British Medical Ultrasound Society BMUS do not mention Podiatry on their site, the Consortium for the accreditation of sonographic education (CASE) do include the Royal College of Podiatry. In writing this article I spoke to one of the representatives of the Royal College of Podiatry Specialist Advisory Groups which covers MSK and ultrasound. There is concern of the growing desire to offer sonographic investigation and the diversity of training is at the centre in terms of standards. Podiatry is just one profession that has a history of development through ‘see one, do one teach one’. Indeed this is how progress is often made. It would come as no surprise to learn that formal sonographers are not best pleased that other clinicians are undertaking a skill that has taken them considerable time to train. The P.G.Certificate leading to competency in sonography is accessible but takes 2 years. As with steroid injections and expansion of scope, the problem lies in mentorship. Indeed this is one of the downsides of Independent Prescribing.
Regional blockades
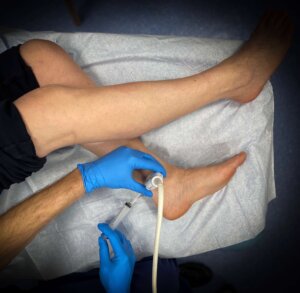
Injection by guided scanning. Courtesy of Chan T 2021
Chan et al 2021 published the first UK guide to sonographic guided injections. The quote from their paper highlights the importance that sonographic guided therapy contributes to patient safety and that training is included within the surgical training programme.
“The use of regional anesthesia in podiatric surgery has long been established and well recognized to provide excellent surgical anesthesia and effective postoperative analgesia, which is ideal for ambulatory day-case surgical procedures in patients who opt to stay awake. … it is ideal for patients with significant co-morbidities who may pose a challenge and an increased risk with general anesthesia.
As part of the surgical training of a podiatric surgeon in the United Kingdom, the ability to administer regional anesthetic blocks is a core skill to include ankle and popliteal blocks as part of the complete perioperative management of the patient. This perhaps is what makes podiatric surgical practice unique, where the regional block is in most cases, surgeon administered.” (Chan et al 2021)
Sonography guided injections will ultimately provide an alternative to nerve stimulated regional anaesthetic blockades. Podiatric surgery has led the way in day care foot surgery for larger complicated surgery in the UK as well as developing anaesthetic techniques without heavy dependence on medical qualified anaesthetists being in attendance for over 30 years.
Focus on podiatric ultrasound use

Ultrasound in podiatry survey
In a study carried out in February 2021 by ConsultingFootPain (CFP), of 113 podiatric clinical responses to an on-line survey, 14.5% held an official sonographic course qualification; 47.5% directed ultrasound through a radiology pathway having used their IRMER qualification. 37.4% directed their imaging as requests through other personnel (medical or podiatric). Although not by any means an equitable comparison with the Siddle official paper which is an important reference, those who attended a formal CASE course equated to 15.8% (Siddle et al 2018). The values quoted here include both short and full courses. In terms of those podiatrists surveyed, CFP n=113 and Siddle n=284.
Training has always come from a wide range of methods and Siddle explored these from manufacturer’s courses, to on-line, in-house mentorship and organisation led. As to the legal requirement and hitherto features of protecting the patient there are two overriding elements. Firstly the equipment used should be tested and shown to meet standards. The dangers of using such equipment near other medical devices for example might be a consideration. Medical equipment cannot be sold for use if risks override concerns for patient safety.
However, ultrasound used as an imaging tool for those without training in diagnosis poses a different concern. Judgement based on ultrasound gives rise to determining pathology. The decisions arising from such determination could be harmful to the patient. In podiatric circles this might involve undertaking surgery to the tibial or peroneal tendons based on incorrectly reading of the image. The other scenario is undertaking an injection to provide anaesthesia and incorrectly identifying the nerve for a vessel or tendon. The growth of steroid placement into joints around tendons could well be included in risks where the clinician was untrained to a standard appropriate to the technique intended. The serious risks from steroid injections in joints has been reported albeit rare (Posmyk et al, 2019)
Using qualified personnel

Shutterstock.com
The use of qualified radiologists or radiographers with sonographic skills forms a different category. The report and discussion of findings provide a useful multi-disciplinary skill arrangement. Access to on-line images via a Picture Archiving and Communications Systems (PACS) type arrangement is valuable as this enhances educational understanding of soft tissue problems. Furthermore, allowing a patient to visualise the screen and discuss the pathology heightens their compliance. Compliance is one of those areas where patients need to take their condition seriously.
Qualification to act upon an official report from a qualified person contrasts the difference in the actions taken by the ‘untrained’ sonographer. We require training and qualification for surgical management. Podiatric surgeons will also use secondary imaging to validate and justify interventions based on reasonable grounds, provided consent is optimised. Carrying out steroid infiltration is altogether different as the sonographic technique and the therapy are combined at the same appointment. In this case there would no time for reflection based on the results unless imaging had been undertaken at a separately.
Results from the ConsultingFootPain survey
 The groups targeted included:
The groups targeted included:
- Podiatrists from NHS and independent sectors (37%).
- Those designated as extended scope podiatrists (41.4%).
- Academic podiatrists not fitting any other category (<1%).
- Specialist podiatrists entitled as non-surgical consultants (4.5%).
- Podiatric surgeons (14.4%)
When using ultrasound as a diagnostic tool, 67.3% confirmed use and 32.7% used ultrasound in different ways as mentioned above such as therapeutic interventions. Research institutions as expected recorded a low 2.6% use, while the NHS and independent sector were more equally distributed between 46.8 and 50.6% respectively. Siddle et al reported 71 and 40% respectively. It would be reasonable to assume that NHS imaging may well be more accessible but this may not account for an expansion of independent ultrasonic units purchases. It is asserted that growth is continuing exponentially and any new study might wish to consider such change.
Use and frequency of ultrasound in practice
When it came to identifying how ultrasound was used. Of 166 responses, injection placement accounted for 35.5%, interpretation of tissue pathology for 44.5%, determining vascular flow 15.6% and research purposes 4.2%. The frequency of use ran to 84 responses accounting for daily use 45.2%, weekly use 32.1%, at least once a month, 16.7% and less than once a month 6%.
There is sufficient evidence to suggest that extended scope (MSK) podiatrists and those in the independent sector utilise ultrasound diagnostics more than we might have appreciated. Data from 2018 and 2020-21 is helping podiatry demonstrate the expansion of scope in one section of our work. Never has there been such an important time for podiatrists to extend their responsibility. To reduce strain on the NHS, to provide conservative care as early as possible, to avoid surgery and to ensure that patients are provided with the best foot health education.
Legal thoughts and regulation
 Returning to the comments on legal requirement. Evidence should provide the gateway in how regulation should proceed. Regulation must not limit the opportunity of quality care delivery where regulation serves little purpose. This is no better exemplified by podiatric surgical training. It should be remembered that pointless regulation based on paternalistic views are both costly, has no scientific meaning and limits beneficial expansion. Nonetheless standards do need to be considered in respect to ultrasound. This is no better contrast than with commercialism associated with foot pressure analysis systems and provision of orthoses.
Returning to the comments on legal requirement. Evidence should provide the gateway in how regulation should proceed. Regulation must not limit the opportunity of quality care delivery where regulation serves little purpose. This is no better exemplified by podiatric surgical training. It should be remembered that pointless regulation based on paternalistic views are both costly, has no scientific meaning and limits beneficial expansion. Nonetheless standards do need to be considered in respect to ultrasound. This is no better contrast than with commercialism associated with foot pressure analysis systems and provision of orthoses.
The fact that there are concerns amongst those who have qualifications in the area sonography form the best group to take advice from. At present information sharing and guidance perhaps remains slower than ideal. Nonetheless in a modern world of accountability, clinicians must develop their practice with integrity and ideally shoot for the highest standards and training. If there is a balance to be met then it is hoped this will have greater clarity than the guidance often given by H.M Government!
Future evidence gathering
A new study is being designed through the Glasgow Caledonian University and it is important that this is supported. You can email researcher Andrew J Brown abrown70@caledonian.ac.uk or Dr Ruth Barn ruth.barn@gcu.ac.uk
Declaration
This article is an independent paper without sponsorship. The data was derived without ethical approval and serves as a snap shop guide only. The views held without reference are those of the author. For formal advice, it is important to refer readers to their professional body for guidance. All locations and respondents are anonymous and derived from external social media podiatry sources (77%) and the CFP newsfeed (23%). The Siddle paper is an open-access paper.
I am grateful to Mr Jai Saxeby for his advice and guidance in the preparation of this article. The Siddle et al 2018 paper is highly recommended as an important resource. For those reading this online article, active links will take you to some of the key sites mentioned by abbreviation.

You can download a PRINTABLE PDF copy for your CPD file HERE. Hyperlinks may disappear. The paper and article are slightly different for format reasons. Reading score = 41
![]()
Siddle, HJ, Patience, A, Coughtrey, J, Mooney, J, Fox, M, Cherry, L. Survey of ultrasound practice amongst podiatrists in the UK. J. Foot & Ankle Research 2018, 11:18 https://doi.org/10.1186/s13047-018-0263-4
Posmyk L, Kilmartin, TE, Coutts, A. Rare but real. Post injection infection. Podiatry Now 2019. 22(3): 8-13
Chan T, Wilkinson A, Hendrick S. A technique Guide in Ultrasound Guided Regional Anaesthetic Blocks. J.Foot & Ankle Surgery 2021:1-7
Why not read Podiatry as a career choice?
Thanks for reading ‘Extending the Scope of Podiatry’ by David R Tollafield
Published by Busypencilcase Communications. Est. 2015 for ConsultingFootPain


Trackbacks/Pingbacks