We need to help patients understand more
Part of Tom’s concerns have been that he has had a number of surgeries without any fuss. So, when armed with all the information why did his private hospital want to repeat tests when they had been done before? In fact they wanted to charge him when he was called back? Why when so close to surgery was he rejected and referred back to the general hospital? Against these delays – why when he was suffering was he bounced back and forth with no action?
Tom, aged 80, illustrates the frustrations of disappointment at being cancelled and becoming overwhelmed by the machinery of health service admission policy. He had been experiencing problems with revision toe surgery for several years. Originally the outcome from his surgery had been satisfactory after his original plastic joint was removed for an arthrodesis procedure (see the image of the plate and screw fixation below).

Golf activity makes a good assessment of foot health
His original story was published 4 July 2021. Problems with the arthrodesis procedure is fairly uncommon but then all surgical procedures have their weak spots. Tom’s second (revision) surgery had not gone that well. He started to notice a dark pigment in the skin of the left, operated foot and symptoms had not been relieved as he has expected. His expectations had been disappointing and he gauged this by his ability at golf, now reduced by the number of holes to 50%. This story is about unexpected delays and frustrations. I met with Tom over coffee on one of the hottest days in the calendar and he opened up his folder containing his notes and various results and some ECG traces.
Three years after Tom’s revision surgery
By April 2022 I asked if he had had any set backs after his original revision in 2019.Until nine months after surgery Tom’s toe was improving. Then it deteriorated.
 “There is dark colouration under the skin with a purply colour. Pain is reported in the arch and on the outside of the ankle. I’m struggling to walk and regretting having the surgery. I cannot wear some of my shoes and the toe sticks up by 5-7cm.”
“There is dark colouration under the skin with a purply colour. Pain is reported in the arch and on the outside of the ankle. I’m struggling to walk and regretting having the surgery. I cannot wear some of my shoes and the toe sticks up by 5-7cm.”
Clinician Comment
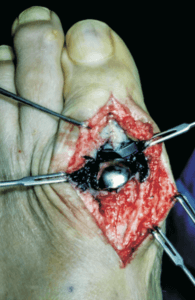 Common problems include movement of screws, fracture of a screw or loosening. He might have a break in the metal plate. The staining described can be associated with metallosis. Allergy to the metal is rarer. Metallosis is usually reported with implants containing metal and plastics. The figure (Courtesy Podiatry Institute 2017) shown is a combination which resulted from a toe implant rather than a plate (Vanore & O’Keefe). However I have certainly seen metallosis in plates for toe joint arthrodesis and the metal components in implants. Owing to the skin being thin the colour can be alarming. When I met Tom finally after he had the metal work removed he recalls no information about the findings at surgery. I would always suggest this is something to ask for.
Common problems include movement of screws, fracture of a screw or loosening. He might have a break in the metal plate. The staining described can be associated with metallosis. Allergy to the metal is rarer. Metallosis is usually reported with implants containing metal and plastics. The figure (Courtesy Podiatry Institute 2017) shown is a combination which resulted from a toe implant rather than a plate (Vanore & O’Keefe). However I have certainly seen metallosis in plates for toe joint arthrodesis and the metal components in implants. Owing to the skin being thin the colour can be alarming. When I met Tom finally after he had the metal work removed he recalls no information about the findings at surgery. I would always suggest this is something to ask for.
Delays, frustrations and protocols
Tom was able to have surgery in a local private hospital and after somewhat of a delay, largely around the post-covid period of NHS chaos he was all set for surgery. Use of the independent sector is far from new and today the NHS rely on the additional capacity for elective procedures – these are operations with low risk.
Tom is a fit looking man who betrays his age in looks and movement by ten years. He knows he has slowed down and that large garden he once cared for is a little too much – so downsizing made sense. Now he feels disappointment perhaps more about the delays and set backs. Relocation from a larger property also meant having to change doctors although a letter to chase up delays finally resulted in surgery but not in the originally planned independent hospital.
We looked at some of the background problems. On the surface it appeared his delays were partly beaurocratic confusion, Covid and to a lesser extent moving house.
The NHS uses private hospitals in the UK for large amounts of orthopaedic, and in some cases podiatric care. My views on the NHS have been published May 2022 (The Dying Healthcare System) elsewhere on this site as the current NHS descends into an inefficient public service industry unable to deliver the nations’ healthcare effectively and efficiently.
Tips on Health Issues
Tom takes a standard diet of heart medication common to many men over the age of 60. However this generally is not a problem if all is stable as the medication reduces those latent risks from further heart disease. The process of ensuring patient safety is paramount. After all, it is embarrassing to lose a patient on the operating table through poor assessment of a patient unsuited to surgery! There are two elements: the anaesthetic and the surgical recovery. Tom slips into the first of these two concerns.
Pre-admission
Patients are usually provided with a pre-surgical assessment close to the intended surgery date. An experienced nurse will undertake a questionnaire and arrange blood tests and an ECG for certain categories of patients. Tom’s ECG threw up two problems; a previous myocardial infarction and a right sided nerve conduction problem called a bundle block.
Myocardial infarction (MI)
The heart is essentially muscle and pump with its own blood supply (coronary vessels). If these vessels are blocked then part of the muscle can die off which affects the contraction (squeezing pressure). Death of muscle due to blood supply depletion is called infarction. In most cases patients recover fully and with medical supervision. Sometimes MI may not even produce symptoms and is picked up by a routine ECG trace.
Bundle Block
Right branch bundle block (RBBB) means the nerve conduction required to stimulate the heart squeeze is faulty so that part of the heart (ventricle) does not contract and allow the squeeze pressure to work as well. The reasons for RBBB are given below, but RBBB occurs more frequently in men than women. Here are some causes of RBBB.
- Heart disease from high blood pressure
- Chronic obstructive lung disease or COPD
- A blood clot in the lung, otherwise known as a pulmonary embolism
- Right-sided heart failure
- Cardiomyopathy, which is a disease of the heart muscle
- Idiopathic fibrosis or degeneration in the right bundle branch
- Cardiac surgery
- Myocarditis, which is an inflammation of a membrane surrounding the heart
- Aberrant ventricular conduction
- Congenital heart disease
- Coronary artery disease
- Heart attack
- Surgical procedures on the heart
As the right side is more intimately connected to the lungs receiving renewed oxygen, any defect can give rise to problems especially under general anaesthetic (GA). GA based procedures introduce drugs that alter lung function so breathing is assisted during an operation. Under conditions where someone has no medical problems the risks are very small. The reverse is true with medical problems especially cardio-respiratory disease (heart-lungs).
The difference between a private hospital and NHS General hospital
There can be no doubt that these are not small concerns from a patient’s perspective. Tom is a highly intelligent man who can process complex technical information. We as in the healthcare profession, are poor at providing digestible information in many cases. Surgeons perhaps, are worse than physicians if I am allowed a generalisation. Reliance on stock publications often removes the human element and the surgeon expects an information sheet to make up for the lack of explanation.
Tom contracted Covid at one point and so an additional delay was likely. Still, he remained in the dark about being rejected as he reasonably deduced he had had surgery under GA before without concern. The explanation above provided the core rationale and tends to be related to GA-based procedures. However, independent (private) hospitals do not have an intensive care bed or facility. The NHS and general hospitals are the only places where 24-hour staffing and funding allow sick patients to be admitted with all the support facilities the independent sector cannot provide.
Specialised intensive care
It is important to appreciate that some independent hospitals have intensive care but this is based on strict protocols (rules) allowing care of the dying from cancer. Some high-staff-resourced care is undertaken, but not for unknown medical complications. Since the NHS decanted care to independent hospitals, rules were implemented to ensure that certain categories were screened and rejected if a potential risk was identified. Tom fell into this category but was not given a sufficient explanation. The confusing feature is that private care (paid for by patients or insurers) can circumvent the NHS protocols, which appear at odds when defining risk. Curiously, he was offered to follow-up tests at his expense despite him being an NHS referral. Cross-over costs are often refused by the NHS so recovery by the independent hospital might have been in place.
The anomaly of private cases not following the same strict rules as the NHS referrals to those hospitals still exist. It comes down to the admissions (screening) nurse, the medical advisory committees and ultimately the hospital manager, who can change the course of someone’s admission. Most consultants will review any concerns raised and admission will not go ahead, particularly where the consultant anaesthetist is correctly involved.
To some extent, spinal blocks provided by anaesthetists and limb blocks, as performed by podiatrists, can avoid general anaesthetic, which immediately reduces the risk posed by the type of problem Tom had. A spinal anaesthetic was discussed but rejected by the anaesthetist who had found Tom a poor candidate from previous experience.
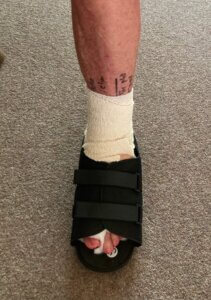
Tom’s foot after surgery (with permission)
And finally, the revision surgery itself
Tom’s foot was now 8+ weeks after all the metalwork had been removed. The scar was fine and flat, and his foot, even on this August day when temperatures hit 28C, was not swollen abnormally. The skin was not discoloured as it had once been. The toe was stiff and slightly shorter than the right foot big toe. From a clinical point of view, all looked sound, and the procedure had achieved its aim – but not from Tom’s viewpoint.
The fact that matters were not necessarily better disappointed Tom, and we meet the ‘grey area’ associated with repeat (revision) surgery.

Risks from surgery
One surgery is always best. I know this as a foot surgeon and patient, having been at both ends of the scalpel. The tissue is virgin except for any pathology found during the operation. The wound is sewn up (sutured), and this is when matters start to follow their own course. The material used can set off a reaction and increase inflammation as the body fights to absorb material designed to be left in. What do you really need to know after bunion surgery?
The benefits must be weighed when we drift to a second or third surgery. Could I be made worse? Should I stick with what I have? The first surgery created scar tissue, and the virgin anatomy has now changed at the bone, joint and skin level. The nerves – which are critical, can change the messaging service to the brain. Numbness is the best and most common example. However, some nerves are designed to recall pressure, some heat and cold, and others pain. In other words, there are specialist nerves. Nerves interact with chemicals, and these chemicals are produced by the body within the surgical site associated with inflammation.
Adapting after surgery
We alter our way of walking after foot surgery, which is not always good. Pain comes from walking differently, and revision surgery takes longer to recover. As we age, we heal more slowly than when young. When Tom and I discussed the potential for revision surgery not always working, he did accept this. However, I know all patients retain positive hope and always keep an optimistic outlook.
Tom made the right choice and has shared his experience openly, which hopefully will help others understand not all is as it appears. Taking that step for further surgery needs more information and explanation than the first because false hope is misleading.
Thanks for reading ‘Delayed big toe surgery!‘ by David R Tollafield
David is a former podiatric surgeon working in the NHS and independent sectors.
Why not read more about the bunion (hallux valgus) and behind the scenes on this website or buy the e-book/paperback by the same author.

Published by Busypencilcase Reflective Communications Est. 2015


Trackbacks/Pingbacks