Seeking a reason for hidden pain
The author discusses his own clinical experience associated with the condition of Complex Regional Pain Syndrome which he calls ‘pain with failed healing after injury.’
We all know about pain – it hurts, but what if that pain does not subside, or pain medication does not help, then we consider that we have failed to heal after injury. This article will introduce you to a painful condition also known as a pain ‘syndrome’. The blue links in this article support more detail around the subject. Some articles do contain adverts.
Causes of pain
Pain arises because of insult or injury. A process known as inflammation kicks off, and clinicians recognise redness and swelling as part of the so-called cardinal signs. These had fancy names all in Latin; dolor, calor, rubra and turgor. Calor we recognise as heat and dolor as pain, while rubra is redness and turgor swelling. A complex pain syndrome affects specific regions of the body. The limbs, in particular, are targets, so hands, feet are high on the locations impacted. During the American Civil War, when humankind realised the lasting effect of the aftermath of the battle carnage, nerves were first associated with unexplained pain. As with any road map, we start with the site of injury and the nerves. The route taken by pain messages is far from simple because it passes through the spine from where it travels to the brain for processing. However, the spine can resend messages back to the limb, confusing the brain and bypassing the control centre. Because the sympathetic pathway is involved, we have associated the pain syndrome with this part of the nervous system. The truth is that we are still learning about the brain and all of its oddities and it is not quite as simple as pain nerves are also involved with the process. The skin sweats more than expected in severe cases belonging to the sympathetic system’s control over the sweat glands.

likened to a tap, pain fails to turn off after an injury. No pain – extreme pain
Failed healing
With injuries, we cut our skin, and it heals. In normal circumstances, we would expect that to be the end of the story because there is nothing to show if pain continues despite all other evidence to suggest matters are normal. This is the single reason why hidden pain is the most difficult to deal with.
Once the skin repairs, all that we see is a scar. We fail to see the area below the scar where the process of healing continues over several months. Scar tissue is deep as well as superficial. As children, we liked to show off our injuries through the road map of scar–tissue repair. Once the skin is covered with new skin cells, the pain diminishes rapidly as nerve endings are covered. But the injury settles slowly in some cases depending upon where that injury arises. It seems that the part of the sympathetic nervous system is at fault. The so-called pain tap does not turn off. Chemicals flood the area, local pain nerves are excited when they should have settled and these add to both symptoms that alert us from further damage and bring in the new building process expressing a signal that we are not progressing as we should. It is often weeks before we realise that all is not well. Many health professionals will use those hallowed words – “things will settle but it takes time”. At this point, you realise that you are not healing after your injury.
The primary medical and surgical care on the battlefield was horrendous. Lack of knowledge about infections, microbes, and dressings was often relegated to limb amputations in the infancy of management. If the bullets and debris of ballistic missiles failed, then crude surgery torn into muscle and nerves. Reflex sympathetic dystrophy or RSD was one of several names given to this constant pain. Still, as with many medical conditions, it has been refined over time through various names, including causalgia, to become complex regional pain syndrome or CRPS. The syndrome element suggests more than one set of symptoms or relationships that overlap with similar conditions. Medicine is heavily sprinkled with similar conditions called syndromes.
Clinical experience exposes the ignorance
My own baptism of fire
In the 21st century, we still meet CRPS, but injuries to hands, feet, legs, and arms are the most frequent location away from the battlefield. While no longer suffering from the wild nature of the battlefields, modern surgery can still set off CRPS, a little akin to post-traumatic stress syndrome. PTSD was the shell shock so vilified within the British Army during the 1914-18 conflict that some 300 men were executed for cowardice amongst other crimes. A man, woman or even a child can experience an injury that sets off the syndrome. Records even show that some mastectomies can result in CRPS. A seven-year-old child knocked his foot and developed CRPS in his big toe. Although this was one of my earlier experiences, it was not the first. As a junior (podiatric) surgeon (FRCPodS), I saw my first CRPS in 1986 after being referred a 14-year-old patient with the after-effects of a failed ingrowing toenail surgery. She developed pain after I revised the sides of the toenail. Eighteen months later, having researched the subject and shared this with my patient, the patient’s GP was disgusted that I had broken the code of ethics. My crime had been to provide mother and daughter with the efforts of my research. I sought an opinion from the orthopaedic department, who believed that the nail had not been appropriately treated and operated on this poor young girl three more times. Upon their discharge, the young girl came back to me.
Somewhat disturbed by these medical failings, I came across a friendly anaesthetist specialising in chronic pain because we shared the same operating theatre. So my baptism came about in a way I could never have realised, and until I retired, my passion for the condition has never wained. Sadly I went on to see more CRPS during my career, and my caseload recorded higher numbers of CRPS than my colleagues because I was so focused on the diagnosis. Some accused me of over counting, but anyone with a series of unexplained pain that continued for more than 2 months, was categorised at risk.
Has medicine reflected on the condition?
Medicine now recognises the condition more receptively and with an improved balance of sympathy. Still, as a whole, the condition and the effect of having a fractured wrist or the simplest of surgeries can provoke a holocaust of inflammatory symptoms. I attended meetings for patients and colleagues and ran tutorials and seminars. One with an actor trained in medical care delivery. How to handle distraught patients and advise them of the journey they would most likely follow. Even I was surprised to learn symptoms could be so severe as to increase the sensitivity of the female erogenous zone, as one professor of pain management from Bristol advised. When I discovered one of my patients with heightened arousal, embarrassment had stopped her from informing her husband, who now listened with shock. However, my abiding memory came from the very worst that the condition could deliver, which is worth telling.
Advanced stage complex pain syndrome
 For more than 20 years since my first sufferer opened my clinical door and mind, I realised several stages from mild to moderate and then severe. The latter creates wasting of the limb, arm or leg, hand or foot. The skin changes colour and texture. Pain arises through a rush of air, a sudden sound or injudicious movement of the limb affected. The nature of pain is hot to burning. As one sufferer said at a conference I had organised, ‘pain is like putting your whole arm in a bucket of hot water and not removing it ‘. Causalgia is a term used to describe this side of the syndrome. In the advanced stage, the limb becomes stiff through disuse, and those with the worst symptoms end up in wheelchairs. And so to my story…
For more than 20 years since my first sufferer opened my clinical door and mind, I realised several stages from mild to moderate and then severe. The latter creates wasting of the limb, arm or leg, hand or foot. The skin changes colour and texture. Pain arises through a rush of air, a sudden sound or injudicious movement of the limb affected. The nature of pain is hot to burning. As one sufferer said at a conference I had organised, ‘pain is like putting your whole arm in a bucket of hot water and not removing it ‘. Causalgia is a term used to describe this side of the syndrome. In the advanced stage, the limb becomes stiff through disuse, and those with the worst symptoms end up in wheelchairs. And so to my story…
Asked to help a woman by a different pain specialist to the one I had first worked with, I was asked if I could make a splint to prevent the inevitable contractures. I advised against this, but both his patient and he persisted in persuading me. I discussed this with my own anaesthetist, who would have to knock my patient out for us to get anywhere near her limb. Despite years of experience casting feet and legs, I brought in an orthotist to take a mold of the lower limb. Once the plaster cast had been removed, it would go back to his work station, and a plastic shell would be vacuum formed into the finished article and refitted. Once in place, the splint would hold the limb, preventing it from bending and the tendons tightening.
As the anaesthetic took effect, my anaesthetist and I watch with amazement as the limb straightened from a furled up part of the anatomy with its mottled hue to a fresh colour that looked pink and healthy together with a straight leg. If I had been religious, I would have credited this with a story from the Christian bible. ‘Jesus saith unto him, Rise, take up thy bed, and walk,’ from John 5:8 – but sadly, no such thing arose. Once the anaesthetic, which works on the brain, wore off, the leg reversed its pattern. The leg bent, the skin changed tone and colour. We stood astonished as this act. Had it been an experiment, it would have failed to pass ethical approval. But, unfortunately, it was no experiment but a directed part of management. The pain that accompanied this patient’s return to consciousness was amplified three-fold, and we had to shoot her up with morphine. Much to my unhappiness, we had to repeat the whole process to fit the device, which was an absolute disaster for the same reasons. I could explain this event in physiological scientific terms, but I desire to make people aware of the condition as a lay article.
Have we learned from these salutary lessons?

As I was writing a new book called Foot Health Myths, Facts & Fables – Podiatry Reflections, I researched current stories. Much as I am against amputation, a case was cited by the Daily Mail online, a British tabloid that applies a sizeable latitude at times when it comes to podiatry. A 19-year-old sued the NHS after being treated for an ingrown toe (2012) and had an amputation that the tabloid suggested resolved her pain. The report by Kate Pickles in 2016 arose 30 years after my initial case. It is newsworthy for one reason alone. That reason exemplifies the fact that simple treatment can lead to untold consequences, and as clinicians, we are often helpful at supplying the best management. The surgeon who causes the problem is not doing so out of negligence but is often insufficiently trained to make any difference. The pain specialist might be an anaesthetist or a rheumatologist, but the reality is that the box of tricks available comes with a simple message.
Trial and error!
In truth, treatment starts with the earliest of suspicions leading to a presumptive diagnosis. The patient must be briefed immediately and counselled of the likely route without false promises. After that, there is a wake-up call; medicine might not believe you. Friends think you are shamming. Employers believe you’re pulling a sicky! Marriages start to creak with destructive forces of altered sensitivity.
The pain management ladder starts with simple analgesics but soon requires supplemental medication to manage discomfort. Gentle physiotherapy is essential, and the use of the limb should be encouraged as rest, and lack of movement is a disaster. Contractures arise because of our reflex to guarding against pain. We stop moving. The skin must be trained and desensitised by light pressure build-up. The brain must be fooled, and mirror therapy can help (also see Sayegh 2013). Psychology is essential, and any input from favourable cognitive treatment is necessary. Group therapy is vital as a help network. Sleep management is critical to ensure the brain can cope and depression is averted. Surgery plays a minimal part, while amputations are not advised. The Daily Mail might sell more papers because of a small silly innocuous ingrowing nail costs NHS as a headline. Then there is the narrative of the prosthetic limb redolent of soldiers returning from Iraq and Afghanistan, which offers a metaphor for the battlefield. It is the less savoury side of journalism!
Healing after injury requires us to manage pain
Indwelling nerve stimulators are now an avenue to managing pain, and this method will grow as technology allows for smaller indwelling devices and keyhole surgery. The modern toolbox must include counselling, pain management, movement, positive psychology, and available support.
This year I decided to write a short (fictional) story about Anna Taylor called ‘The Withered Hand’, a copycat of Thomas Hardy’s ‘The Withered Arm’. Hardy came from Dorset, which happened to be the location of the young woman associated with Kate Pickle’s article in the Daily Mail Online. As a retired clinician and journalist, I thought it was appropriate to put the condition of CRPS in the context of inadequate NHS resources and t the consequences of suicide. Many sufferers dream of this and amputations. If I have been harsh in my criticism of opportunistic journalism, Pickle’s article does take you through some of the realities of CRPS and is worth reading.
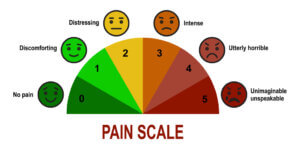
CRPS will range from level 1 to level 5 in the worst cases
The sad truth
The truth is that while NHS centres can provide excellent services, even before the ravages of Covid-19, the chronic pain clinic was understaffed and under-resourced. Of most concern is the fact that delays in treatment make the condition harder to manage. The best advice I can give is to seek a pain specialist early and not be advised by a non-specialist, GP or surgeon, to see how it goes and take strong pain killers alone. As a foot surgery service, we buddied up with physiotherapy and the pain specialist service. We followed their protocol to manage CRPS early so that we had already tried to minimise the condition’s progress by the time they saw the consultant. As a result, our case numbers were not significant. Together with extended consulting clinic times in which we provided counselling, we had a modicum of success, and many cases of mild CRPS improved. That said, I was always unsure what the NHS accountants thought!
![]()
Sayegh SA, Filén T, Johansson M, Sandström S, Stiewe G, Butler S. Mirror therapy for Complex Regional Pain Syndrome (CRPS)-A literature review and an illustrative case report. Scand J Pain. 2013 Oct 1;4(4):200-207. doi: 10.1016/j.sjpain.2013.06.002. PMID: 29913636.
Bruehl S, Chung OY. Psychological and behavioral aspects of complex regional pain syndrome management. Clin J Pain. 2006 Jun;22(5):430-7. doi: 10.1097/01.ajp.0000194282.82002.79. PMID: 16772797.
Additional (USA) source – National Organization for Rare Diseases (NORD)
Other articles on this site
Acute and Chronic Pain
Painkillers for Foot Conditions
‘The Withering Hand’ is one of eight short stories available as an e-book or paperback from AMAZON books by David R Tollafield.
Priced at £4.99 and £7.99
My small pre-published book Myths, Facts & Fables is FREE can be downloaded when you sign up. The full version is now available in paperback from AMAZON BOOKS
Thanks for reading ‘Pain with failed healing after injury’ by David R Tollafield
Written for a lay audience, hyperlinks used in this article allow for greater in-depth understanding.
Published by Busypencilcase Reflective Communications Est. 2015

Published 9th September 2021


Trackbacks/Pingbacks