Ever wondered why your feet smell?
I consider the subject of smelly feet and the home truth in this article. The condition makes up one of the biggest ‘ugh factor’ for feet. The smell provides a perception of an unsavoury condition. By and large, smelly gungy feet are not that common. People care about the odour in feet as much as they do around armpits so it is unlikely that this is down to poor hygiene. There is usually a good reason why feet might suddenly appear unsavoury. Part of our role is to investigate the problem and then manage it.
See the self-help guide at the end
Are sweaty feet due to poor hygiene?
Few things put people off more than the thought of sweaty feet. According to one source, your feet have more sweat glands than any other part of your body – even more than your armpits. “It’s entirely normal for your feet to produce more than a pint [568 mls] of sweat in any given day, says Dr Juliet McGrattan in an article for netdoctor”.The term for smelly feet is bromidrosis. The term for excessively sweaty feet is hyperhidrosis. But contrary to popular belief it’s not the sweat that causes bromidrosis. Foot odour arises from the bi-product that bacteria produce, offering four prominent smells: sweaty, cheesy, vinegary and cabbage-y.
Methanethiol is a key component in the flavour of cheddar cheese. Acetic acid is a result of sugar fermentation — and is better known as vinegar. Byproducts associated with rot, such as propionic acid and butyric acid, can leave feet smelling like rancid cabbage. The most common foot-related chemical, isovaleric acid, is responsible for the smell we call “sweaty. “Our noses are up to two thousand times more sensitive to this chemical than the others, and many of us can recognise it even at the slightest concentration.”
 Bacteria live on the skin of your feet and digest the sweat, producing chemicals thought to be the cause of the smell. The sweat glands are also active in the hands as well as feet. The value of sweat, up to a point, allows some grip and traction as the skin is not smooth.
Bacteria live on the skin of your feet and digest the sweat, producing chemicals thought to be the cause of the smell. The sweat glands are also active in the hands as well as feet. The value of sweat, up to a point, allows some grip and traction as the skin is not smooth.
Sweat glands
There are 250,000 sweat glands in the feet. Some sources suggest our sweat glands, known as eccrine glands, may exceed McGrattan’s statement and therefore the real quantity of sweat produced will depend on weather, activity or stress levels to start with. Nerves and hormones regulate this activity. Men sweat more than women.
Poor hygiene adds to the build-up of skin squames offering greater bacterial opportunities. However, increased sweating requires temperature, exercise, stress and can be affected by medical drugs and chemicals as in foods. Increased sweating may require medical intervention. One condition that is not so uncommon is pitted keratolysis. We have met the word ‘lysis before which means to break down.
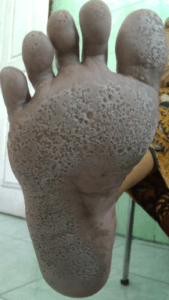
a severe case pitted keratolysis (Wikipedia)
Corynebacterium or Kytococcus sedentarius are causes of this intense smell. The appearance is pronounced with pits made within the top layer of moist skin turned white. Contact with the skin and aroma make this highly offensive. Similarly, interdigital sweating (between toes) can lead to bacterial breakdown as in the case of toe irritation. If you suffer from pitted keratolysis this will need medical management. A culture to identify the organism and antibiotics to remedy the problem.
 Medical reasons for sweating
Medical reasons for sweating
- Injury
- Infection (Tuberculosis)
- Emotional (psychological /mental/pain)
- Diabetes
- Increased thyroid activity
- Cancers (blood/lymph)
- Skin – pitted keratolysis, tinea pedis (athlete’s foot)
Why are my nails dirty?
There are several good reasons why your nail is discoloured. Forget what happens to your fingernails when you work with dirty tools and products. Unless you are in the habit of going barefoot, or your shoe leaks when out walking, or is affected by the dye in your shoe – there is a cause. Toenails are no longer a valued part of our body as our fingernails are. Nails are weapons and tools of the trade on the four limbs.
Unlike our pets, we cannot scratch our ears with our feet in adulthood. The nail, like the skin, is made from a protein called keratin. This is the same substance discussed earlier with corns and callus. Keratin is hard, resistant to water and keeps out those nasty bacteria and viruses. However, the nail ages and thickens with use. The quality changes in density and structure. A sporting or occupation such as dancing may rip a nail after prolonged pressure and initiate the process of repair and thickening. The nail lifts at the end and starts to separate. The gap left between the undersurface of the nail and the skin leaves an entry to another bug – fungus. Think about stale bread forming penicillin-like mould. Dark, warm and moist environments encourage the growth of fungal spores.

smelly feet and the home truth
Fungi with names
We, podiatrists, love names and if we can grow a fungus bug from a nail sample we are thrilled and can tell our patients they have trichophyton rubrum or some other wonderful foreign name. Of course, names are in Latin or Greek! Fungus the Bogeyman, inspired by the artist Raymond Briggs comes to mind. Perhaps we should talk about mycoses as fungal infection is a mycotic infection as we see bacteria being a bacterial infection. The brown, yellow and even blue-green features are just bugs taking up their new home. They are opportunists as they see a chance for starting a family. As far as health is concerned fungi (mycoses) are not likely to endanger healthy humans. The nice look no longer looks so nice. Podiatrists used to reduce the keratin to treat these nails but today they should only do so with masks, respirators and with drills supported by dust extraction because those fungi spores can find their way into the lungs and that is no longer acceptable.
Cross-infection
Cross-infection is how we pass bugs from one person to another. We think of hands and of course breathing out germs. Closed spaces with poor ventilation add to the problem of inhalation. Using a nail file that has been contaminated means you push the same bugs onto the new host. The idea of cross-infection is well known and this is why we wash our hands as we do not know what we might pass on. Again, Covid-19 has shown that those with the poorest health are at the greatest risk from cross-infection. But here is an interesting fact – in cases of clean surgery, facemasks have not always been seen as valid at protecting against post-surgical infection. It would be a brave person to take avoiding masks as a valid rule in this new age of rising infections.
Do you have to be an athlete to get athlete’s foot?
Skin can become infected with a fungal infection but the appearance is different from nails. Nails also make a good substrate for bacterial growth while skin behaves differently. Again the foot needs to create the right environment for fungi. Athletes commonly have skin problems assumed to be associated with mycotic infections. The heat and moisture produced by exercise activity can be impressive. Without the flow of air – some shoes now have holes to help – heat build-up requires the body to sweat. This moisture pools and soaks back into the skin causing softening. Athlete’s foot, often known as Tinea Pedis, forms small blisters called vesicles which are itchy and can spread. In science, we talk about the power of hydrogen or pH. The sweat can change its pH. The more hydrogen (H2) the more acidic a solution, the less H2 the more alkalinic. Sweat increases to help cool our skin temperature. The downside to this is that the foot becomes more alkalinic and prone to alter the types of bugs grown, attracting insects we don’t want in our floral garden.
We find the alkalinity in sweat helps bacteria and therefore we don’t want to attract anything that disturbs our balanced skin flora. Keeping the skin healthy without being too dry or moist is important. The oily nature of skin protects our skin as polish protects the bodywork of a car. In poor health, the skin flora can change opening up the risk of other bugs affecting the skin. Healthy skin has a coating of friendly bacteria. Staphylococcus epidermidis, known as commensal flora, affords protection. Think of flora as a nice flower bed with mixed colours attracting bees. Now reverse that thought and say you don’t want the bees to be attracted. The problem with fungal infections, like bacteria, fungi like an alkaline medium and so bacteria and fungi can work together.
The skin is soggy, macerated (fluffy-wet) and has an unpleasant odour, but this is bacterial. However, treatment as athlete’s foot should be considered together with improving the air circulation to allow this to dry faster. Sandals and open designed footwear work best in the right environments.
Self-help Guide
Sweaty feet are usually unrelated to poor hygiene alone and may have more to do with a medical problem. Managing bacterial activity is essential, but the primary casualty is footwear. Good hygiene is still essential if this problem persists.
Basic questions
- How long have you suffered?
- Is the foot itchy?
- What does the skin look like?
- Where is the problem – between the toes, under the foot?
- Are you in good health
- Do you take medications already which might have brought on the condition?
- Do you suffer from anxiety?
First steps
- Change your shoes regularly and ensure they are allowed to dry if the inside is soaked with sweat
- Check the shoes do not leave pigment or irritate the skin i.e cause inflammation with a border. some shoe pigments and chemicals can cause allergies as in dermatitis.
- Try to air your feet as much as you can and remove socks. Wool is better.
- Use an antiperspirant on your feet after washing
- Hot working environments create problems as do warm floors.
- Use the right footwear for your occupation.
- Punch holes in the sides of shoes to allow more air
- Lightly dust with an anti fungal powder allows prevention and offers early management if the condition has a fungal cause. Wash the powder off regularly
- Dry feet with a hair dryer and ensure the gaps between the toes are dry before using socks and shoes
- Try hot and cold contrast baths
- Anti-odour insoles may be helpful which include cedar or activated charcoal. Available from pharmacy & internet outlets
Contrast Baths: Contrast baths involve a rapid change from warm to cold to help open up and close the tiny capillaries (blood vessels) in the foot. Warmth causes these small arteries to open, which cold causes them to close. This rapid opening and closing of blood vessels near the site of your injury creates a pumping action that’s thought to help decrease swelling and inflammation around injuries. Decreasing the swelling and inflammation helps alleviate pain and improve mobility.
Risks of Contrast Bath Therapy : Contrast baths carry no risk when performed correctly what ensure that the water is used at the correct temperature. The main risks are: burns from water that is too hot and skin damage from water that is too cold. Avoid in limbs with poor circulation and in chilblains without medical (podiatric) supervision.
Ask your pharmacist about:
- antibacterial soaps, powders, and creams
- special foot deodorant
- medicated insoles for your shoes
- antibacterial socks
Pitted keratolysis is one of the chronic conditions and should be treated medically. If the condition is managed this is fine but continued problems need the advice of a podiatrist or dermatologist. Prescription medications may be required which are safe and appropriate with guidance from medically trained professionals.
Reference
McGratton, J 28/12/20 Smelly feet treatment and prevention tips. Accessed 8/2/22
You can also read my article on kidneys and salt regulation on this site and flat feet.
Urine Holds the Secrets of Health and Foot cramp is there a cause
****
Myths about other foot concerns in ‘Foot Health Myths, Facts and Fables’ which is FREE to download by signing-up to my regular newsfeed (go to ConsultingFootPain.co.uk) The book is also available from Amazon.

Sign-up for here my regular FREE newsfeed
Thanks for reading “Smelly feet and the home truth” by David R Tollafield for consultingfootpain
Published by Busypencilcase Communications Est. 2015




Recent Comments