Giving advice on-line as a podiatrist
 Giving advice on line as a podiatrist is not something we have ever covered before on this site. In this article the subject is the ‘corn’ and the ‘bunion’ is given as an example. following one reader’s request for advice. In this short article I am covering more about what information I believe is reasonable to provide on-line via written communication.
Giving advice on line as a podiatrist is not something we have ever covered before on this site. In this article the subject is the ‘corn’ and the ‘bunion’ is given as an example. following one reader’s request for advice. In this short article I am covering more about what information I believe is reasonable to provide on-line via written communication.
All advice has to be based on information provided by the respondent and does not replace the final consultation resulting from a clinical ‘real life’ examination. The following areas will be covered.
- Is this free or is payment required?
- Documentation
- Style of reply
- Advice given
- Methods used
- Caveats
 Bonus and benefits
Bonus and benefits
Clearly since March 2020, and after a viral infection, lockdown and tiers, we have had to adjust our clinical attitudes. Web based consultations are very much in their ascendancy. By on-line I mean e-mail communication only not to be confused with telemedicine and so there is no face to face or voice to voice contact. For most practices there will be a worry about litigation and who pays. Think of it another way. Give something back to the community and use the method to advance and promote your practice. This was certainly my key message in my previous book, Selling Foot Health as Podiatry.

How to go about on-line advice
Written information and visual material helps guide readers and patients so DO provide advice. Set out the limits for advice given and state what is free and what will lead to an charge. The following information given in this example of a real case was fully consented.
Is this free or is payment required?
 I try to make it clear what can be offered and how information might be used. My site is FREE but consent is still important.
I try to make it clear what can be offered and how information might be used. My site is FREE but consent is still important.
Set out your terms
Even if you don’t publish your terms for on-line queries, write them down as a guide so that you can refer back to, dated and if necessary send them to the correspondent. My own e-mail site is reserved for people enquiries alone. It is useful to keep this type of enquiry separate from your main email address. I used my special e-mail address myfootjourneys@mail.com and I check it once a week. My website is set to picks up comments and queries as well as filtering spam rubbish. I ask correspondent authors who write to me to let me know what happens so I can follow this through and share it with readers. The deal is simple. I’ll help you but let me share anonymously. That bit is important and protects people. No names are ever used and I often suggest people provide me with an anonymous name they would like to use as it makes writing more personal. I then ask for their consent in writing. If you have a practice you can use the information in your promotional blurb which carries a good deal more weight if someone replies that it was useful.
ZOOM
History of Present Complaint
Information & correspondence with the real patient in this article
Glad to be of help. Age is useful as it puts an idea on the physiological changes we all undergo. Happy to chat. Ping me a messenger text when you are ready but my website will give you some information to allow you to consider pertinent questions. Your feet by the way are by no means bad I can assure you.
Visual material to assist make the diagnosis
Observation examination (visual photos supplied)
Ask for visual material, ideally good quality well lit pictures. The following three photos provided by Linda (anonymous) are reasonable shots and provide clarity of the key lesions.
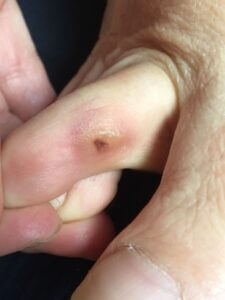
right second toe corn
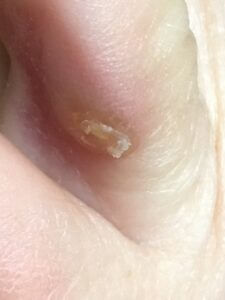
Left 4th toe corn
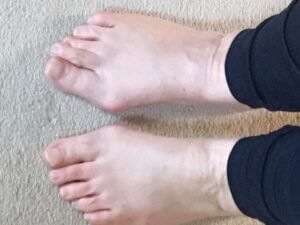
hallux valgus
Clinical observation on Linda B (medical terminology)
Lesion R/2nd Well established with extravasation undebrided. Overlies right second IPJ condyle. Compressed joint by first toe + 15 degrees late onset deformity.
No sinus suspected and dorsal callus ridged emphasising direction of compression.
Lesion L/4th Well established with thickening of main layer and flaking of top layer of epidermal cells. No underlying bursa suspected. Compression again on the lateral side of the foot caused by increasing width of foot due to hallux valgus.
Advice offered to Linda
From the information provided you have late onset bilateral bunions. This probably means that the angle has increased with time and has been present for longer than you may have been aware. The corns are simply a reflection of pressure at two distinct points; the second and fourth toe – one on each foot. I will attach labelled diagrams to show you the underlying mechanics at each joint. Your understanding of the geography of these bones will help establish the prognosis.
Pressure exerted by the widening foot as you have commented relates to both the bunion and your skin responding to growing pressure. Corns form where pressure is greatest. Callus is an earlier presentation of pressure and so both co-exist. The second toe is inflicted with deeper damaged. This is attested by the blood coloured change which is loss of blood and stains as it clots (extravasation) under the skin.
Corn plasters
As a rule, plasters contain salicylic acid paste. The concentration is low and designed to break the layers of skin (epidermis) down so that the hardened area flakes away. Although plasters detested by podiatrists, the skin can respond when used early on in its formation. Some sites on the foot benefit more than others such as the sole only if pressure is not excessive.
 Information provided by the author to a patient-reader query as part of online advice
Information provided by the author to a patient-reader query as part of online advice
A is the direction of push against the second toe due to the bunion
B is the point where the toes (narrow arrows) converge at the condyles (top diagram) trapping the skin in between. Corn is shown in magenta
The aim of management is to a) improve the skin b) remove the pressure c) correct the cause.
The dangers of corn plasters are that they can set up inflammation and in a small number of cases damage the skin and deeper structures of soft tissue. This can also lead to infection between toes on account of the increased moisture and heat. Bugs love this environment. The skin can be improved but it will need professional reduction (debridement) to remove and assess the extravasation present. I doubt a sinus (hole) is present but a professional would identify and manage this first. Removing the pressure is achieved by two further methods. Identify shoes that make matters worse and avoid these. Soft stretchy unlined leather and fabric uppers will reduce the effect of the bunion and pressure. You can use silicone sleeves to reduce the pressure when in shoes. The silicone allows the pressure to absorb through the material rather than the skin.
Conservative approach
A six-month approach to debridement may be all that is required. Use foot cream locally massaged into the skin and us the protective sleeves. These strategies will inform you if this is sufficient. The option to return to former footwear has to be determined based upon your progress. I would not use the corn plaster method as these lesions (any skin problem or change) have progressed beyond their capacity for any value.
Longer term options
If the lesions do not settle, matters worsen, then I would advocate considering having the bunions corrected to narrow the foot, limit the inter-toe pressures and advance your ability to use a wider range of shoes. My website and publications are reasonably detailed on the management of hallux valgus. I have just updated this one with you in mind – bunion. There is another surgical method that is popular and this is called Osteotripsy or minimal incisional surgery (MIS). With MIS the surgeon makes a key hole and the condyle (see illustrations) are shaved down. This is done in a day case theatre, under local and you rest for 24 hours and can start to get around. The first surgery deals with more of the problem but has a longer recovery period. The MIS might work and even if it doesn’t you can still have the bunions corrected.
In the UK the only people who provide foot operations are podiatric surgeons or orthopaedic surgeons who specialise in feet.I hope this helps. These formal notes expressed can be shared should you need to seek the help of a general podiatrist or GP. Provide Name & Qualification and Registration number for formal reports.
 Caveats
Caveats
Most queries will come through mail addresses or via websites. There are both pluses and minuses…
I make it clear I do not offer clinical consultations but if you are a busy practitioner then how much time you are willing to offer will depend upon your own viewpoint as a business. It is good to have a range of help material loaded to your website as you can direct a client to this resource. If not use this site or some of the other sites that are run professionally. My site is updated regularly and monitored. The more information you provide, the more likely a patient will want to see you personally.
time invested is business created
How far you go will depend on the foot problem and your interest. Many call this probono. For the most part you will be considering the patient or correspondent as part of triage. It is important to say what limitations exist with the information provided. Ask only once for more information then terminate further correspondence if the correspondent is unhelpful or a poor historian. Always be professional and polite but firm. A common request comes from a person who is unhappy with another practitioner. If this is the case do not enter into dialogue or comment about another person. You do not know what went on and the information is unhelpful and offers a red flag for withdrawal.
Many foot conditions are so complex that it is not possible to provide meaningful assistance and you can invite the correspondent to make an appointment or see their own GP where in the UK advice is free. Do not seek to promote business unfairly. Trolling is common and any such correspondence should be rejected without a reply and entered into spam.
Don’t miss my second article planned covering on-line consultations this Spring
Thanks for reading ‘Giving advice on-line as a podiatrist’ by David R Tollafield

Published by Busypencilcase Reflective Communications Est. 2015 for ConsultingFootPain
Why not sign-up to regular reflective podiatric practice newsfeeds today


Recent Comments