What are falls and who are the elderly?
I watched my father fall! There was nothing I could do as I was too far ahead of him. We had just returned from our first meal out since Lockdown. This was also my first visit to see him as he lives nearly 200 miles away and he had deteriorated. At 92 years of age one might well expect a risk of a fall. He was using a single stick and walking at his slow pace. Read why this happened in this article?
Today’s article is all about falls the elderly and what we all need to know. The more I dived into the subject of falls and the elderly, the more my interest and enthusiasm peaked. When trying to make sense about the effects and risks I had written an earlier article in 2019 entitled Avoid broken bones at home . The intentions behind this article is to provide more facts and advice. We should all review our ideas about falls in the elderly and what we need to know to help our elderly citizens.
Flesch readability score is 65 suggesting easy read
The first sign: Falls increasing!
This was not my father first fall. I had a fear that these events were increasing. I fixed an appointment to see the GP (with my father) and it was clear she neither had time or the skills let alone resources to deal with the subject of ‘falls’! Kathryn Anderson (2008) writes;
It is known that approximately one in three people over the age of 65 living in the community will fall each year. This figure approaches one in two by the age of 80, and fall rates are even higher for residents of nursing homes and those in institutions.
The concept of falls and the elderly therefore is far from new. But there is a wider impact – Falls in the elderly. As a podiatrist I know of the interest that some of my own colleagues have. There is passion amongst many who care for this age of the population spectrum. I have seen my own wife fall several times and I managed a slow dive off a wall myself last month. I crashed into our BBQ! Indeed it was as if I was in slow motion. The younger model that I am no longer am would have been different. Damage, graze on leg, bruised skin, hurt pride and one broken BBQ leg! Repair is slower as we age. The leg of the BBQ was quick to fix in contrast.
NICE Guidelines
The government backed body that looks after evidence that treatment both works and is economically viable has published their NICE guidelines. These show in their 2013 publication (reviewed in 2019) that the interest, recognition associated with falls in older people must be assessed and prevented. The subject might appear dust dry. The implications for carers, the family, let alone multidisciplinary teams, is profoundly important.
Understanding more about falls and the elderly

Monkey Business images/Shutterstock.com – doctors do not always have time despite trying to be empathic
I needed to look further at this subject as clearly I was not up to speed as I should be. Now I needed to focus on my father. Anderson reminds us that fall rates are higher for residents of nursing homes and patients in hospitals fall with devastating consequences. Leslie Kernisan writes about the type of things doctors should check for, but it is the deeper narrative of her internet article (link), Better Health While Aging, that grabbed my attention as I searched (24/8/20) for information accessible to the public for my September Autumn Newsfeed. Dr Kernisan makes quite a statement.
“Busy doctors may not be thorough unless caregivers are proactive about asking questions. Most doctors have the best intentions, but studies have shown that older patients often don’t get recommended care. By being politely proactive, you can make sure that certain things aren’t overlooked (such as medications that worsen balance).”
This statement seemed to reinforce my early comment about my father’s doctor’s response.
What is a fall?
I define a fall as an uncontrolled moment when the body loses balance with unintended consequences. The effect can leave an immediate injury or a delayed effect that erodes confidence.
Falls are the leading cause of accidental death in older people. Anderson (2008) goes onto to highlight the hidden costs for the individuals in terms of depression, loss of confidence and even mortality. Injuries might well be visible or obscured by the risk of internal bleeding. Fractured bones are common in an aged person because their bones are weaker due to poor resilience.
Explaining the mechanics of a fall

Flareimages/Shutterstock.com
My father turned quickly and lost his balance. He failed to control his position as someone younger would. So what’s the difference between him and a younger person?
His spine has increased its curve as well as losing space between each vertebra. As the spine shifted forwards (see diagram below) this had the effect of moving his centre of gravity forward. He needed a stick to increase the base of his feet. The wider his base the better his stability. His movements are plodding, and therefore slow. This means he can control his forward progression but he must concentrate carefully. Loss of concentration can cause a fall.
His ear provides balance, but aging has reduced this information and he is deaf. Reflexes provided by his tendons are equally less effective. Information to the brain arrives from the tendon sensors. The speed (reflexes) of making adjustments is now slower. His eyesight is affected by aged macular degeneration so his peripheral vision is poor. His neck suffers from cervical spondylosis so it is stiff and movements are slow. Both knees have been replaced with new joints. Although he has moderate pain he copes with this. The surgery will have altered his joint awareness (proprioception). One foot is painful and therefore again so that there is a reluctance to respond quickly due to the altered sensory nerves in the sole of his foot plus discomfort.
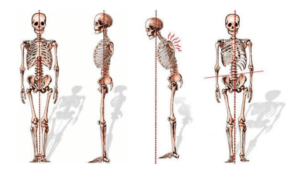
Centre of gravity shift with the spine as shown. Taken from https://www.columbiaspine.org/condition/spinal-deformities/
With loss of spacial awareness, reduction of reflex conduction and poor muscle balancing in his posture, the process of wasting takes its effect. The upright posture of the younger man he was has altered. What a young person might consider easy, someone of older age will find more difficult.
By twisting to see an object it is easy to see how balance is lost and recovery is poor. The injury awaiting will rely on the direction of contact, the forces involved in that movement and the surface against which the person falls. These are low impact forces and yet poor quality bone will yield at its weakest points; shoulder joint, clavicle bone, neck of the femur and through the hip joint. If an outstretched arm makes contact with the ground then the wrist and shoulder will fracture taking the brunt of that impact.
Injuries
Concussion, fracture, bleeding into muscle are all potentially serious. Recovery is very slow and even during recovery problems can arise. Hospitalisation is not ideal for the elderly. Hydration as in insufficient drink, poor eating habits and kidney problems can lead to confusion. The brain is affected by these simple changes. In many cases falls lead to early elderly mortality and happen when in hospitals.
Things to check for with relatives
 Reaction to drugs and prescriptions should be checked. Patients should take no more medication than required. An update on medical health is important. Eyesight and glasses should be managed through regular appointments with an optometrist. All old medicines and out of date food should be discarded. Small nutritious meals are important and plenty of water should be used daily to maintain hydration. Toilets should have easy access. Damaged paths and walkways should be repaired and made safe.
Reaction to drugs and prescriptions should be checked. Patients should take no more medication than required. An update on medical health is important. Eyesight and glasses should be managed through regular appointments with an optometrist. All old medicines and out of date food should be discarded. Small nutritious meals are important and plenty of water should be used daily to maintain hydration. Toilets should have easy access. Damaged paths and walkways should be repaired and made safe.
Deteriorating medical problems
Dementia, confusion and urinary tract infections. Poor mobility aids or lack in using such aids to prevent falls. Around the home all objects should be within easy reach and climbing onto ladders, reaching upwards, lifting heavy objects should all be avoided. All elderly people need a network of friends and people around to help where family are not close. Contact through a reliable neighbourhood watch or emergency fall call buttons attached around the neck at least provide some comfort when people live alone.
 What can I do to prevent a fall?
What can I do to prevent a fall?
I turned to the AgeUK website and felt that this provided some guidance. As a close relative I know I must do all I can for my father. He is important to me and the link to my past. The link to the ageuk site deals with elderly fall prevention and reminds us that “some health conditions, medications and footwear can affect your ability to stay steady on your feet. You might not notice your health changing as it can happen gradually, so it’s important to have regular checkups so any issues can be picked up before they cause a fall.”
Our Future Plan
 For my sibling and I, we have plenty to do to ensure our father has the best quality of life. I set out a plan and copied my father into this as well as discussing my ideas with him together with my sister. We have Power of Attorney for health but also his consent so that is the first place to start. Involving parents and ensuring they understand choice is important
For my sibling and I, we have plenty to do to ensure our father has the best quality of life. I set out a plan and copied my father into this as well as discussing my ideas with him together with my sister. We have Power of Attorney for health but also his consent so that is the first place to start. Involving parents and ensuring they understand choice is important
(1) To discuss openly with GP and patient (with son) current concerns.
(2) Instigate all support where possible to retain both independence and retain living in his current home.
(3) Take action to minimise falls.
(4) To ensure best support of patient with relatives and friends.
Doctors in the NHS have little time to spend on social chit chat and one has to balance up the value of consultations and what they are prepared to do. My plan was not even discussed, the room needed to be ‘vacated’ for someone else. As someone who was a consultant in health care I know the limitations!
David is a retired Consultant Podiatric Surgeon and now independent author and freelance journalist you can read more about him or connect to his website he is also on Facebook@david.tollafield or Twitter @mypatientjourneys
Thanks for reading my article ‘Falls the Elderly and what we all need to know’ by David R Tollafield
Published by Busypencilcase Reflective Communications Est. 2015

September 2020

Recent Comments