A naval bone and the Duke of Edinburgh?
How pain stopped a young woman from competing
 Foot pain and the Duke of Edinburgh might seem completely unrelated but in fact this story is relevant; to undertake the Duke’s Award the respondent needs to be foot pain free. At the grand age of 99 the Queen’s consort, husband and confident died. It seems fitting to write at the time of his passing of an event that shaped one young person’s desire. That desire was to complete the Silver element of the revered Duke of Edinburgh Award (official website). This is ConsultingFootPain’s tribute to the Duke which coincides with Foot Health Week. The article is packed with great links to help you explore this problem and follows on from my article ‘Time to challenge the flat foot’.
Foot pain and the Duke of Edinburgh might seem completely unrelated but in fact this story is relevant; to undertake the Duke’s Award the respondent needs to be foot pain free. At the grand age of 99 the Queen’s consort, husband and confident died. It seems fitting to write at the time of his passing of an event that shaped one young person’s desire. That desire was to complete the Silver element of the revered Duke of Edinburgh Award (official website). This is ConsultingFootPain’s tribute to the Duke which coincides with Foot Health Week. The article is packed with great links to help you explore this problem and follows on from my article ‘Time to challenge the flat foot’.
- Pain and the Flat foot
- Navicular bone pain
- Duke of Edinburgh Award
Pain and flat feet
 Nothing can be more exciting than see someone in pain make a full recovery. Rachel wanted to undertake the prestigious Duke of Edinburgh Award. This challenging award had been going as long as I had been living. The conditions for the awards are activity based. Rachel was aiming for the Silver element. At 17 years of age this lovely student was not doing so well with her foot, and in particular her arch. The appearance of the flat shape was misleading as the pain centred around one bone – the navicular. This sits in the middle foot area. Of most importance this bone is the anchor point for the big foot tendon that holds up the arch. The enlarged navicular bone is may an extra bone or os tibiale externum.
Nothing can be more exciting than see someone in pain make a full recovery. Rachel wanted to undertake the prestigious Duke of Edinburgh Award. This challenging award had been going as long as I had been living. The conditions for the awards are activity based. Rachel was aiming for the Silver element. At 17 years of age this lovely student was not doing so well with her foot, and in particular her arch. The appearance of the flat shape was misleading as the pain centred around one bone – the navicular. This sits in the middle foot area. Of most importance this bone is the anchor point for the big foot tendon that holds up the arch. The enlarged navicular bone is may an extra bone or os tibiale externum.
A flag ship bone
The Latin os tibiale external makes it sound grand but the navicular bone is boat shaped hence its name and ‘os’ implies an extra bone. The Duke was of course well known to the navy and so the link is apposite. Doubtless he would be interested in the foot analogy but the navicular really is a flag ship bone as it makes up the important midfoot joint with similarities to the hip joint. The bone (the talus) that fits into this saucer like shape cup of the navicular is rounded. If this part of the foot becomes unstable it upsets the mechanical balance of the foot. You can read more about the midfoot in an earlier article. The Third Ankle Joint
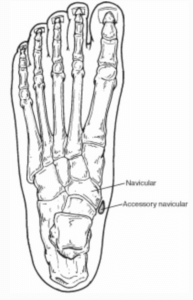 As a (podiatric) foot surgeon I had to decide whether the bone, which bulges normally in all feet, was a cornuated navicular, which implies enlarged and fused together. Rachel’s navicular was larger than normal. We have extra bones all over our feet, each given the prefixed ‘Os’. Some of these accessory bones are more common than others. The foot appears flat as the bone sticks out and is irritated by shoe wear and rubbing during walking. Additionally the powerful muscle tendon that inserts into the enlarged end (tuberosity) is displaced slightly and therefore alters the foot’s mechanical efficiency. The arch appears lower because of the failed mechanics. Surgery is straightforward and one I am always confident to help improve. I shaved the excess bone away and tightened the big tendon so it would work better. This was a procedure called a Kidner operation.
As a (podiatric) foot surgeon I had to decide whether the bone, which bulges normally in all feet, was a cornuated navicular, which implies enlarged and fused together. Rachel’s navicular was larger than normal. We have extra bones all over our feet, each given the prefixed ‘Os’. Some of these accessory bones are more common than others. The foot appears flat as the bone sticks out and is irritated by shoe wear and rubbing during walking. Additionally the powerful muscle tendon that inserts into the enlarged end (tuberosity) is displaced slightly and therefore alters the foot’s mechanical efficiency. The arch appears lower because of the failed mechanics. Surgery is straightforward and one I am always confident to help improve. I shaved the excess bone away and tightened the big tendon so it would work better. This was a procedure called a Kidner operation.
The naval or boat shaped bone ignored
Flat foot problems will always remain a challenge for podiatrists. It is dependent on many factors such as the natural shape of the foot shape and secondary problems associated with medical diseases. These diseases include diabetes, leprosy, rheumatoid arthritis although there are others. The foot specialist’s nightmare will always be managing obesity, soft tissue deterioration and foot weakness. Younger patients will do better if they are lighter and healthier. Probably the worst condition is posterior tibial dysfunction syndrome or PTTD. The posterior tibial tendon is large and can easily inflame causing fatigue, flattening of the arch especially if it tears. Another patient of mine called Gracie had had PTTD to start with. It had been missed at a point that her pain could have been assisted. Doctors and even podiatrists may learn about such conditions but they are rarer than bunions or hammer toes and heel pain. Examination while not that hard can be a problem if a doctor cannot make time to look at the foot, let alone examine the function, shape and movement carefully. Pressures of the modern GP surgery, to say nothing of Covid-19, contributes significantly to missing these musculo-skeletal problems. All too often drugs like ibuprofen are substituted as a mode of treatment. Like the ingrowing toenail and treatment with antibiotics, the anti-inflammatory is often seen as a Smartie like placebo even if it is given for genuinely well-intentioned reasons. If used for more than five days without benefit, few musculo-skeletal pains will subside without a clearer diagnosis.
Posterior tendon pain and tears
PTTD had three main stages. For the most part Gracie’s third stage is rare, but middle stage tendon tears are not uncommon. For the most part I pick up first stage PTTD, where I can do something. Podiatrists with a keen interest in biomechanics and musculo-skeletal specialisation can avert further problems. I am fortunate where I worked that a very large community of GPs do not hang onto patients and would send them to me, or another foot specialist. Orthoses and arch supports form a significant part of dealing with long term prevention of PTTD. Females are always compromised by their desires and passions for ever new fashion designs which simply do not suit the wearing of material which takes up room in a shoe. Men fair better but PTTD is not a condition to take lightly and this is where orthotic management does make a big contribution even if it does not straighten out the arch.
Self-help
You can help yourself with two basic approaches to help navicular pain. Protect the bone using a donut pad or check to see if the shoes are causing a problem and replace these. Most people undertaking the Duke’s Award will wear stout boots. If the bone is prominent the skin may rub. Blisters are not uncommon but if you experience pain that radiates back into the ankle then seek help.
The donut pad
Make a pad out of felt and shape it like a round donut with a hole. You can stick the pad directly to the skin if you don’t have any skin problems or the the inside of the shoe. The felt should be 4-7mm thick (around 1/4 inch) to protect the bump. I prefer to make my own pads as they flatten in time and make the fitting and wearing more comfortable. A fresh pad is easily made up as needed. The pads are good for activities but the skin should be spared long term contact. Foam can be used instead of felt. For longer period of protection stick the pad inside the shoe rather than the skin. If the foot fails to improve seek a podiatrist’s help.
The Duke of Edinburgh Award

http://www.jsu.edu/news/articles/2012/04/two-miss-jsus-receive-duke-of-edinburgh-award-medal-from-prince-edward.html Alabama USA
As a foot health journalist I cannot do justice to the Duke’s memory and years of service to the United Kingdom. It is best left to great authors and biographers who have the depth of knowledge and correct perspective. The Duke touched people’s hearts all around the world (picture USA) and his so called outspoken comments made him unique rather than represented a man who was careless for the sake of being rude. The Duke’s story will remain the centre of attention for some time to come.
Madeline Grant writes for the Daily Telegraph and in the Saturday 10th April (2021) edition she writes passionately about the Duke and his award. “The D of E gave a much-needed injection of the old Swallows and Amazons spirits into school – which were too often excessively cautious, health-and-safety obsessed environments.”
Grant appears to have undertaken the Gold award as she injects a personal ring side description;
“…we learnt practical skills like map reading, cooking over an open fire and camping – but also the intangible things too:stoicism, sticking power and the ability to keep going when cold or exhausted.”
Our intrepid Young Award seeker after her surgery…
Rachel completed her Duke of Edinburgh Award successfully. Receiving her warm words in a card thanking me for making it all possible was the best award for me. She collected her treasured Silver Duke of Edinburgh Award as had Madeline her Gold.
Taking on passionate patients and being asked to return them to full function is no easy task. I took on Rachel because she was so dedicated in her quest to complete the award. I admit I was worried. Surgery was a big step to take and she could have been made worse and not even made the goals set by the tasks. Time was of the essence which posed another pressure on me as a clinician. However I felt that as she had already tried the conservative approach and this had failed, that surgery was the right decision. As the United Kingdom laments the Duke’s death we will all celebrate his positive contributions which were not exclusive to our small island.
Thanks for reading ‘A naval bone and the Duke of Edinburgh’ by David R Tollafield

Regular articles on foot problems from a trusted professional site
Published by Busypencilcase Reflective Communications Est. 2015
Published 12th April 2021


Recent Comments