Rachel’s double toe surgery
 A Behind the Scenes Patient Journey Series
A Behind the Scenes Patient Journey Series
In this series we are discussing revision surgery and the first toe, often associated with a painful bunion. The joint surface was damaged but the left side less than the right. Bunions frequently have a loss of the surface of cartilage resulting in stiffness. The surgeon must decide which of the 150+ operations is best suited. In reality, most foot surgeons will probably use no more than six approaches to deal with either the bunion or painful stiff toe. Rachel worked in a pharmacy department. She was 47 and had stiff toe joint pain. Blue writing will take you to different links and help build a picture depending upon the detail you need.
Throughout, clinician comment will elaborate on the storyline. Please read the other cases on ConsultingFootPain as these paint a different picture starting with the Introductory article. Rachel kept her own log and stayed in touch for 6 months between 2017-18. We pick up her story in 2021 after 4 years.
 Her case story
Her case story
2012-2014
Rachel had a painful bunion on each foot. She had the right foot managed first in 2012 and received an implant (plastic hinged joint). Her left foot had an osteotomy (bone cut procedure) in 2014. The right foot had more cartilage damage than the left foot.

Swanson implant (silicone) C/O Wright Medical
CLINICAL COMMENT
It is usual to try to maintain healthy cartilage using an osteotomy. By 2017 her osteotomy was not doing so well and it was clear that a new approach was required. As her right foot did so well she elected to have a revision surgery using the silastic implant. Some osteotomies fail. We don’t have a figure on conversion from osteotomy to other surgery but conservatively this would be estimated at around 5%. Surgery is reserved for when all other treatment has failed, or the joint is irreversibly damaged. Surgical joint management involves the joint being removed entirely and either left with a gap or a spacer being introduced into the gap. In Rachel’s case, the surgeon had to convert the osteotomy to a silastic prosthetic joint.
The day of surgery
Written in diary form
 The operation went well –2nd replacement joint so kind of knew what to expect, best part was the anaesthetic, is it wrong that I find it so relaxing? No pain when I came around. My foot was elevated and I had some kind of bucket filled with ice and water attached to a boot (this filled up with the cold water) so it felt wonderful. I was allowed to take this home for several days which was great for reducing the swelling. Didn’t feel the need for pain medication but took some before going to bed even though the pain was very minimal. The anaesthetic block was still in place. From previous experience the block would wear off during the night and I would be in pain. Stayed at parent’s bungalow so getting to the toilet was a lot easier than having to shuffle on my bum up the stairs. All in all first day and night were comfortable.”
The operation went well –2nd replacement joint so kind of knew what to expect, best part was the anaesthetic, is it wrong that I find it so relaxing? No pain when I came around. My foot was elevated and I had some kind of bucket filled with ice and water attached to a boot (this filled up with the cold water) so it felt wonderful. I was allowed to take this home for several days which was great for reducing the swelling. Didn’t feel the need for pain medication but took some before going to bed even though the pain was very minimal. The anaesthetic block was still in place. From previous experience the block would wear off during the night and I would be in pain. Stayed at parent’s bungalow so getting to the toilet was a lot easier than having to shuffle on my bum up the stairs. All in all first day and night were comfortable.”
After surgery
Day 1
“Foot still very numb, still no pain, but continued to take the pain medication just in case. I could see the bruising at the end of my toes which is to be expected, started to wiggle toes and even wiggle the big toe a little. Having to wear a sexy little blue shoe – not a good look coming up to Christmas, having to heel walk for the first 7 days which I keep forgetting to do. I am not too good at resting either, and so helped parents put Christmas tree up. Stupid thing to do as the foot was very sore by mid-afternoon. I need to remember I only had the operation yesterday – so the foot is now resting and elevated. Feeling a lot better by early evening. Another good night’s sleep on pain meds.”
Day 2
“Uncomfortable morning, feels like the block has really worn off now. The foot feels so stiff and sore. Trying to wiggle as much as I can, not sure if I am supposed to be doing this, but find it helps to loosen off. Had to have pain meds this morning, but all in all a good day.”
Day 3
“Pain very minimal, I wouldn’t call it pain as such, more tingling sensation, and slightly sore. Again felt very stiff and lumpy underneath but from past experience knew it would feel like this. Rested the foot as much as possible today, although I did get in the shower with the leg sleeve for first time today. Can’t say enough how wonderful it was to get under that water. I feel as though I haven’t showered for weeks. The foot pulled a bit afterwards but pain meds kicked in quick. Still having to heel walk which isn’t the easiest thing to do, can’t wait to get the air boot on tomorrow.”
 CLINICAL COMMENT
CLINICAL COMMENT
Showers are not recommended too early because of the risk of falling. Appropriate rails and support are best. You can buy temporary handles to stick on tiles or glass to act as safety grips. A chair that can be used under the shower also helps with foot surgery. A specialised jacket is better than a plastic bag. Plastic bags can rip and also do not have a viable waterproof seal. All our patients were provided with ice (cryotherapy jackets) and plastic covers.
Day 4
“First appointment with the nurse today. Can’t wait to get out of this blue (post-operative) shoe and get the air boot on. Nurse changed dressing, I couldn’t look – I hate the sight of blood so when I saw it all over the bandage it turned my stomach, needless to say that was the worst bit. The wound was amazing, so clean and tidy. Obviously bruising to the toes but such a neat job – wonderful consultant job yet again.
Disappointed – I can’t have the air boot on until my next appointment the following week as I still need to heel walk.”
CLINICAL COMMENT
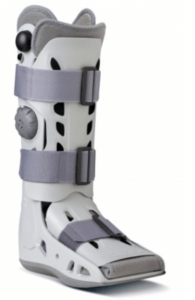 Shoes allow better walking as they are flat and adjustable but they are not intended for heavy use. Large dressings must be accompanied by suitable footwear. The AircastTM boot is a product often called a walker cast. This is made from a heavy plastic 2 piece shell with a hefty sole curved to allow the foot to rock forwards safely limiting the discomfort. Large dressings must be reduced and so too much padding will cause pressure. Rachel describes her disappointment at not being able to use this system as she knows from past experience her mobility will double.
Shoes allow better walking as they are flat and adjustable but they are not intended for heavy use. Large dressings must be accompanied by suitable footwear. The AircastTM boot is a product often called a walker cast. This is made from a heavy plastic 2 piece shell with a hefty sole curved to allow the foot to rock forwards safely limiting the discomfort. Large dressings must be reduced and so too much padding will cause pressure. Rachel describes her disappointment at not being able to use this system as she knows from past experience her mobility will double.
Day 5
“I am back at home today so tackling the stairs, walking sideways up and coming down on my bum. Foot slightly tender today but nothing I cannot deal with. Again having gone through this before I think my brain knows what to expect. Had it been first time round maybe I would be more uncomfortable. In fact I am probably doing too much, the nurse did tell me off (a little) yesterday as she could see I was trying to run before I could walk, therefore lots of rest today, foot up and Christmas movies.
Evening – first time cooking for myself as I have been waited on hand and foot at parents for last few days. Cooking was okay, but standing washing up my foot became quite tender. I elevated the foot on cushions for the evening, but no need for pain meds as I am not good at taking tablets so only take when I am in real bad pain. Had a great night’s sleep in my own bed. The winter quilt was a bit heavy so my foot poked out of the bed most of the night but the cold actually felt good on it.”
Day 6
“Had good night’s sleep, decided to try and walk the dog with my parents today. Big mistake, only out for ½ an hour. My foot was so tight and sore after, then to top it all off I stubbed my toe on a cabinet. Nothing that pain meds couldn’t sort out, but I need to realise my foot needs resting more. Felt very sore during the evening, felt lumpy underneath, but still only felt a bit of discomfort.”
Day 7
“Good night’s sleep again with no pain, still finding the quilt a bit heavy on my foot, I could do with one of those cages to hold the quilt off!!. Did a bit of shopping down the supermarket today with parents. Used crutches so not too bad. I am finding walking around with the shoe on is giving me back ache. Perhaps I am being too cautious and not putting as much pressure on as I should, but I have been told to heel walk for first 7 days.”
Day 8
“Not able to get out today so going a bit stir crazy. Can’t wait to get the air boot on now so I can at least go up the garden with the dog. Missing my long walks with him, I need to stop feeling so impatient. Been trying to bend my toe. It’s so stiff and I have flinched a couple of times, maybe I am best to wait until I go to physiotherapy. Stood and did a bit of ironing. Past day day so trying to walk more through my toes today. They are stiff and uncomfortable but not painful. I do feel it when I eventually put my feet up, it’s like a fuzzy feeling through the whole of my foot, almost like when you have had really bad pins and needles. I feel like I want to bang my foot on the floor to get rid of it, but obviously I don’t.”
CLINICAL COMMENT
Rachel started to improve much as we see in the previous case of Leah. While Leah and Tom had surgical plates, Rachel only has a plastic hinged joint and so she was encouraged to do more to keep the toe mobile. Nonetheless, the warning is to take matters cautiously during the first week.
Six months later
“Foot is fantastic, best thing I did going ahead and having the replacement joint, although I do still get a certain amount of swelling, especially after a long walk, which I am now back up to speed with. I am walking the dog approximately 3–3.5 miles each day. I find it swells up more if the weather is warm, but a bag of frozen peas for half an hour soon settles it down. My foot has gone back down from a size 5 to size 4.5, which makes it easier to buy shoes.”
Four years follow up
“Foot is progressing well, I have to admit it does give me pain at times particularly through the Winter months when my foot is cold. I have at times struggled to walk as it seems to swell up so much so that a few months ago I was going to contact you to get advice on who to see as I felt it may need x-raying. Alongside the pain it does cause me to have problems with my lower back as I am probably not walking probably on the foot at all times due to the pain, it can actually wake me up in the night with shooting pains, not very often but when it does it is very painful.” April 2021
CLINICAL COMMENT
There is no doubt that surgery, especially revision surgery can make the foot sensitive to cold. Strangely feet are almost barometers of pressure change in the weather. The reason for this is that we have a complex pattern of small blood vessels susceptible to constriction and dilation changes. We suffer chilblains when our circulation cannot adapt. Nerves associated with scar tissue also seem to be less able to function and may be akin to dental nerve pain when those fillings are no longer working. Metalwork within the surgery, screws, plates, and anything that is not made by the body will conduct heat and cold differently. The solution is to add insulation to the shoes or socks. Keep the skin supple at all times and never use hot water bottles. Massage is always valuable and works with applying the cream. Medication can reduce shooting pains but stick to paracetamol or ibuprofen initially before working up to stronger drugs that work in the nervous system. Always look to a healthy diet with fresh vegetables and vitamins especially oily fish. Maintain exercise as much as possible to work the leg and foot muscles. Back pain arises because the foot/feet are imbalanced. This can be solved by having your gait analysed by a professional podiatrist and use fitted orthoses. Once these measures have been tried or if symptoms persist, then an x-ray and consideration for the implant to be managed might be necessary.
The two approaches I have used for revision surgery include, (1) remove the implant and leave the space. Or, (2) undertake an arthrodesis. In this case, one needs to follow the case of Tom for all the inherent risks.
Thanks for reading ‘Revision Surgery and the First Toe’ by David R Tollafield
A Behind the Scenes Patient Journey Series
Why not read more about the bunion (hallux valgus) and behind the scenes on this website or buy the e-book/paperback by the same author?

Published by Busypencilcase Reflective Communications Est. 2015
July 2021


Recent Comments