Leah’s Story and her arthrodesis operation
 A Behind the Scenes Patient Journey Series
A Behind the Scenes Patient Journey Series
It might sound all very obvious, but do we get big toe surgery right the first time? Indeed yes this does happen but not always. This series covers different patient stories taken from their own words. All had stiff big toe joint pain. This is Leah’s story. Blue writing will take you to different links and help build a picture depending upon the detail you need. Throughout, clinician comment will elaborate on the storyline.
Please read the other cases on ConsultingFootPain as these paint a different picture starting with the Introductory article. Unlike the other 2 cases in this series, Leah had not had surgery before.
She kept a log from 2018 which she sent to ConsultingFootPain during the course of the first 7 months. This was reviewed in 2021 by e-mail. I joined Leah before her surgery in a UK National Health Service Hospital. Her surgeon provided information that she shared which is not always the case read more about What you really need to know after bunion surgery?– an information article essential for all people undergoing foot surgery to this big toe.
Damage to the first toe joint
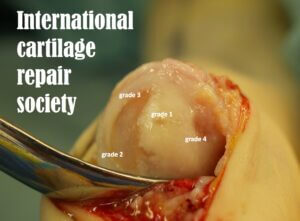
international cartilage repair society score 1-4 as in first toe joint (author)
Leah was diagnosed with a stage 3 joint determined as a hallux rigidus. This typical joint has little space between the bone ends. The surrounding surface has spurs or projections (osteophytes). A damaged joint is used to make some comparison to common findings
She tells her story which goes back to 2018…
“My left bunion was noted 3 years ago by my Australian family. They were astonished that I had not had it removed. The bunion was unsightly and limited my choice of footwear.” The first signs had been 3 years earlier as the feet had become more uncomfortable. They ached after walking even in sturdy walking boots. High heels used for dancing hurt. She tried different shoes then drifted toward felt pressure pads and silicone spacers between her second and first toe; “I arranged to have the operation and was surprised how quickly the appointment came which I had to delay because of holiday plans, at this time my right foot was becoming very painful over the big toe with arthritis. Due to a cancellation, I was able to have both feet done at the same time I would highly recommend having both feet done together.”
The Process of arthrodesis
CLINICIAN COMMENT
While bunion surgery does not require fusion to make it stiff, if the joint is damaged the surgeon is faced with trying to stop movement surgically where conservative treatment fails. The use of splinting, stiff-soled shoes can help. A female patient who is passionate about shoes with heels must be aware that once a joint is fixed, the height of a shoe is determined by the position of the toe afterwards. This position is usually elevated by 5-10 degrees so the toe is deliberately placed slightly off the ground. Leah was provided with a similar device to Tom in order to allow her to mobilise early after surgery. Leah’s surgery was performed under local anaesthetic. This is where she remained awake but as with a dental procedure, her feet were numbed first.
Theatre & surgery under local anaesthetic
 “In theatre a screen was placed in front of me – a calm atmosphere was helped with soothing music and constant reassurance from the staff. I managed to read two chapters of my book. There was no feeling in my feet during the operation, just the sound of the saw and drill. It was all over in less than an hour. I felt calm me knowing what to expect, and told the anaesthetic could last up to 10 hours.
“In theatre a screen was placed in front of me – a calm atmosphere was helped with soothing music and constant reassurance from the staff. I managed to read two chapters of my book. There was no feeling in my feet during the operation, just the sound of the saw and drill. It was all over in less than an hour. I felt calm me knowing what to expect, and told the anaesthetic could last up to 10 hours.
First experiences
“Around 6.45 pm I started to feel the anaesthetic wearing off with some throbbing and by 7.30 pm I took two pain tablets (co-codamol 30-500mg) as the pain was intense. I tried watching the World Cup for distraction whilst lying in bed with my feet elevated. I kept moving my legs which seemed very heavy to ease the pain. I experienced throbbing and shooting pains in both feet so tried to keep my feet elevated. I took more painkillers at 11.30 pm and an hour later felt nauseous with a dread of having to use the bathroom.
I was awake at 5.30 the next morning and my feet were not throbbing so much but still painful. I had a bedside wash and cuppa tea then took 1 tablet at 7.30 am. Again I felt a little nausea but the pain was controlled. I noticed a tiny area of blood on my big toe. A bit of elevation helped using two pillows.”
Day one
Leah slept during the morning of her first day after surgery and developed shooting pains on top of her right foot in the afternoon. A single pain killer worked. Nearly 6 hours later the throbbing started again so she was finding taking the pain medication worked up to its maximum (6 hours) benefit. She was able to wiggle her toes and had a shower with plastic bags. As this was June she spent an hour in the sun. She was even walking without crutches. If you were wondering how she was able to achieve this, well she had slipper casts on she called later called ‘pots’. These casts do not go above the ankle.
One week plus
Leah required no additional pain control and she felt she could stand on her feet without wincing. Sleep had improved and she was now using pain medication sparingly when the feet throbbed, usually in the evening. Her legs were often recorded as feeling tired and heavy. By 12 days she was managing a shower and washed her hair while sitting on a stool again with plastic bags as her feet still had dressings. Her feet tended to throb at bedtime but she did not need pain medication. The next day she found the hot weather caused her restlessness and she had to be careful not to do too much walking. Her check-up was at the 2 weeks mark.
Two weeks
Her feet had been hot with the plaster air shoes but made walking comfortable. A cast cutter caused a bit of anxiety but the noise is scarier than the actual cutter which vibrates and is safe from cutting the skin. “Everyone was pleased with the healing process. I was then able to wear trainers told to walk “flatfooted” with most of the pressure on the heels.” The next appointment was in 5 weeks’ time.
 Her feet felt a lot cooler without the casts and this allowed her to start to massage the scar and bathe the foot. As she was able to moisturise the foot this would help remove some of the dead skin which makes the enclosed foot flaky. The foot had ankle swelling and was bruised on the balls of her foot and one of her toes. The trainers had to be used without laces otherwise it would have been tender over the scars where the incision had been made. By two weeks Leah was more comfortable. She was showering and finding massaging around the scars manageable and using Bio-oil. The skin tapes (steristrips) were no longer required any swelling in her left foot had diminished and the bruising had faded. Swelling did persist around the scar area. Walking was still limited around the house for short periods. Swelling increased when overused. At night there was occasional stabbing pain over the left bunion. She noted that she missed walks and dancing and keep fit classes.
Her feet felt a lot cooler without the casts and this allowed her to start to massage the scar and bathe the foot. As she was able to moisturise the foot this would help remove some of the dead skin which makes the enclosed foot flaky. The foot had ankle swelling and was bruised on the balls of her foot and one of her toes. The trainers had to be used without laces otherwise it would have been tender over the scars where the incision had been made. By two weeks Leah was more comfortable. She was showering and finding massaging around the scars manageable and using Bio-oil. The skin tapes (steristrips) were no longer required any swelling in her left foot had diminished and the bruising had faded. Swelling did persist around the scar area. Walking was still limited around the house for short periods. Swelling increased when overused. At night there was occasional stabbing pain over the left bunion. She noted that she missed walks and dancing and keep fit classes.
Three – four weeks
Leah could walk to the end of my street which was about 100 yards ‘quite easily’. Her left big toe ached in the evening. Now she was nearly at four weeks she started to walk ‘comfortably around town using sandals mostly.’ She was driven to the shops. The swelling was still present and the scar has a faint pink colour which she maintained with Bio-oil daily. Her walking was slower than normal.
Five – six weeks
‘My legs and feet are tired after a walk around the shops, and my feet can really swell up on the wrong shoes. Tender skin over the scar area (thin skin). Bought wide fitting soft sandals. Going for x-ray photograph and final check 9th August.’
 The foot surgeons were pleased with the two feet and x-ray views. She noted that her big toes tended to bend a little to the next toe and swelling persisted around the scar area. Massage was to be maintained. Leah was fortunate as she had retired and was able to swim, cycle and undertake a little line dancing. ‘I love walking but find my feet ache so the distance is limited. Trainers and Velcro fastening sandals though my Havana’s flip flops are comfortable around the house, they also help to keep a space between the big toes
The foot surgeons were pleased with the two feet and x-ray views. She noted that her big toes tended to bend a little to the next toe and swelling persisted around the scar area. Massage was to be maintained. Leah was fortunate as she had retired and was able to swim, cycle and undertake a little line dancing. ‘I love walking but find my feet ache so the distance is limited. Trainers and Velcro fastening sandals though my Havana’s flip flops are comfortable around the house, they also help to keep a space between the big toes
Past the 2 month mark
Today her problem centred around her big toes rubbing. She had a painful ball of her right foot under her big toe due to wearing the wrong shoes. She feels she needed a lot of cushioning under the sole so went back to her trainers. This did not put her off and she embarked on travelling around the coast. ‘Some aching side of balls of my feet and under my big toes. Enjoyed some walking and line dancing. Scars are so faint, very pleased with the whole operation.’ Her next entry showed that her feet and accustomed changes altered frequently.
‘Feet are comfortable but the first toes are raised around their joints causing some friction in some shoes. My flip flops are the most comfortable around the house. This week I wore kitten heels comfortably. My friend has decided to have her bunion done she is so impressed with my surgery.’
Three months
‘Nearly invisible scars,’ were noted. ‘The only problem is my left big toe is rubbing the toe next to it. I have found wearing a silicone toe cap over my toe £1 from Savers is comfortable when wearing closed shoes. I am back to Line Dancing. Feeling good.’ She had a break in Spain during October. ‘Lots of walking just about forgot I had the bunions done wore sandals flip flops high heels dancing, No problems, Pretty Feet!! Continue to massage and moisturise very night.’ Back home now and in regular footwear – ‘Some big toe discomfort in certain shoes and boots better in my widest sizes. I find my toes don’t like the fit of opaque tights. The big toes tend to rub the second toes. Think my feet prefer sandals.’ Then she developed chilblains in November. Of course, it is easy to create this if sandals are used in cold weather. She recorded ‘itchy painful thin skin over the big toes…’ The chilblains lasted 1 week and she thought this was caused by the hot water bottle and walking around London shopping.
A recurrent problem associated with big toes pushing against the second toe kept being recorded as well as ‘finding my toes ache unless I wear cushion or memory soles.’ Leah was followed up in mid-December and had another x-ray and readying herself to go abroad in 2019 on a long haul flight. She flew out in the new year and in February 2019, 7 months after surgery she records in her ‘bunion diary’. ‘Hi just back from Australia, feet ok cycling hiking swimming. Had my assessment in December with photos. The only problem is both big toes lean and rub the second toe making the skin break (not good as I have diabetes type2). I use gel toe protectors to stop the rubbing.’
 By 2020 the UK was hit with the pandemic and so I followed Leah up in April 2021 at just under 3 years since her original surgery back in 2018. Her response by e-mail was encouraging. “David here are my post-surgery answers.” I had asked is she had any setbacks since surgery. “I need to use silicone toe spacers between the big toes both feet, otherwise the big toe rubs the next toe until it is very sore.The first toe both have some arthritis no pain. The procedure was really successful. The only problem re diabetes is cold feet in bed. I can wear any type of shoe, Yes I would have the procedure again both feet at the same time. I can pursue my usual activities, line dancing keep fit class cycling rambling club gardening. Advice to new patients have both feet done at the same time. And a resounding ‘I have beautiful feet now.’
By 2020 the UK was hit with the pandemic and so I followed Leah up in April 2021 at just under 3 years since her original surgery back in 2018. Her response by e-mail was encouraging. “David here are my post-surgery answers.” I had asked is she had any setbacks since surgery. “I need to use silicone toe spacers between the big toes both feet, otherwise the big toe rubs the next toe until it is very sore.The first toe both have some arthritis no pain. The procedure was really successful. The only problem re diabetes is cold feet in bed. I can wear any type of shoe, Yes I would have the procedure again both feet at the same time. I can pursue my usual activities, line dancing keep fit class cycling rambling club gardening. Advice to new patients have both feet done at the same time. And a resounding ‘I have beautiful feet now.’
CLINICIAN COMMENT
Leah had bilateral (both feet) operated on. Her mobility was reduced (35/100) but not critical while her pain score and the impact on her social activities and wellbeing was recorded as 75/100 which is relatively high.
 Two feet are not always easy to cope with at the same time but she had the right mental attitude and did well. Her operation was arthrodesis with plate fixation. It is not unusual for the basic recovery to take 2-4 months and then a little longer for some. Footwear and the female foot is a challenge and Leah certainly appreciates that she needed to be flexible and the seasons could make a difference. Chilblains are something to avoid and relate to cold exposure and certainly rapid heating can lead to itching and pain. When comparing Leah’s case to Tom’s revision surgery there can be little doubt that primary surgery works better and is more sustainable than revision surgery. Secondary arthrodesis can be successful but creates more challenges for the surgeon and patient.
Two feet are not always easy to cope with at the same time but she had the right mental attitude and did well. Her operation was arthrodesis with plate fixation. It is not unusual for the basic recovery to take 2-4 months and then a little longer for some. Footwear and the female foot is a challenge and Leah certainly appreciates that she needed to be flexible and the seasons could make a difference. Chilblains are something to avoid and relate to cold exposure and certainly rapid heating can lead to itching and pain. When comparing Leah’s case to Tom’s revision surgery there can be little doubt that primary surgery works better and is more sustainable than revision surgery. Secondary arthrodesis can be successful but creates more challenges for the surgeon and patient.
Thanks for reading ‘Getting big toe surgery right’ by David R Tollafield
A Behind the Scenes Patient Journey Series
Why not read more about the bunion (hallux valgus) and behind the scenes on this website or buy the e-book/paperback by the same author?

Published by Busypencilcase Reflective Communications Est. 2015
July 2021

Sign-up, stay in touch – download my free book on foot health myths, facts & fables today



Trackbacks/Pingbacks